
I suffered from debilitating migraines for nearly two decades. After seeing 40 doctors, I’ve finally found a $50 cure… I couldn’t believe the results
For nearly 20 years, Rachel Weaver’s entire world was spinning.
In January 2006, the then-31-year-old had just moved to Colorado for graduate school to study writing. But on the morning of her orientation, she woke up with an intense dizziness she hadn’t felt before.
She had been ‘very healthy’ at the time with no pre-existing conditions, so she initially assumed it was a case of nerves.
But she continued to feel unsteady throughout the day with seemingly no explanation. ‘And then for 18 years, it never stopped,’ Weaver, now 51 and author of the memoir, Dizzy, told the Daily Mail.
‘The dizziness would change a little, but for the most part, it was just this very seasick feeling all the time, like everything was moving around me.
‘I started going from doctor to doctor to doctor. No one could figure out what was wrong with me.’
Weaver estimates she saw more than 40 doctors over the next decade, undergoing countless MRI scans, blood tests and X-rays. Finally, an osteopathic doctor diagnosed her with chronic vestibular migraine, a form of migraine characterized by dizziness, loss of balance, nausea and vomiting.
Unlike the 40 million Americans with typical chronic migraine, Weaver rarely had a painful headache – her condition was instead defined by vertigo and a constant spinning sensation. Vestibular migraine affects roughly three percent of the US population, and women are at a five-fold greater risk.
Rachel Weaver suffered from chronic vestibular migraine for nearly two decades before a clinical trial changed her life
After being diagnosed, Weaver was able to control her symptoms for the first time. She utilized a combination of Botox injections every three months, nerve blocks to stop pain signals from the brain every few weeks, rescue medications such as sumatriptan and Toradol, selective serotonin reuptake inhibitors (SSRIs) and physical therapy.
But in 2022, the steady foundation Weaver had finally built crumbled as she tested positive for COVID.
‘I traveled for work and and came back home with COVID,’ she told the Daily Mail. ‘And then everything stopped working – all my migraine meds, everything. It just went back to horrendous, debilitating, all day, every day symptoms.
‘And then I started flinging myself around the country, adding myself to wait lists at all the big migraine clinics or anybody that I felt was maybe researching things or looking at [migraine] from a different angle. I literally had tried everything at this point.’
In 2024, Weaver learned about a clinical trial in the works from Noorda College of Osteopathic Medicine in Provo, Utah. The team was led by neuroscientist Dr Kyle Bills, associate dean of research at the college who started studying chronic migraine to find answers on behalf of his mother.
‘For me, migraine became big because my mother had migraine, and it took a serious toll on her life,’ Bills told the Daily Mail. ‘I think for her, it was a mixture of not just the pain and the loss of function, but I think she experienced guilt of not being around and not being able to do some of the things that she valued.’
Previous studies have suggested chronic migraine, defined by suffering at least 15 headache days a month, are driven by a multitude of factors such as obesity, stress, hormonal changes, genetics and medication overuse, but the picture is still unclear for millions of patients.

Dr Kyle Bills, neuroscientist and associate dean of research at the Noorda College of Osteopathic Medicine, is researching the effect of glucose on chronic migraine
Bills’s team decided to look at an unlikely factor: blood sugar (glucose), which rises and falls based on dietary patterns, exercise and hormones.
‘So many people say, “Oh yeah, if I don’t eat, I’ll get a migraine.” That’s such a common commentary,’ Bills said. ‘And so as we’re doing surveys and having discussions with patients, it was such a constant comment that it forced us to kind of go back as a group and go, “Wait a minute. First off, why is nobody talking about that, and why has no one explored what that probably means?’
Bills explained that when glucose rises, such as after eating, it releases insulin. ‘There are receptors for insulin all throughout the body, and when they’re activated, they pull glucose from the blood into the cells.’
But many patients told the team that if they did not eat or ate certain foods, they would quickly have a migraine after. Bills believes this could be a sign of insulin receptor insensitivity, meaning cells respond ineffectively to insulin, causing glucose to rise and potentially trigger migraine.
The team started by ordering glucose tolerance tests, which measure how well the body processes glucose. These are typically used in pregnancy to detect gestational diabetes.
The tests came back showing consistent trends of post-meal hyperglycemia (high blood sugar after eating). But to look at glucose throughout the day, researchers implemented continuous glucose monitors (CGMs).
Costing between $50 and $100 each, depending on the brand and if it is meant for a diabetic or non-diabetic, the device sticks to the back of the arm with a small needle. It tracks glucose levels in the interstitial fluid between cells 24/7 for about two weeks at a time.
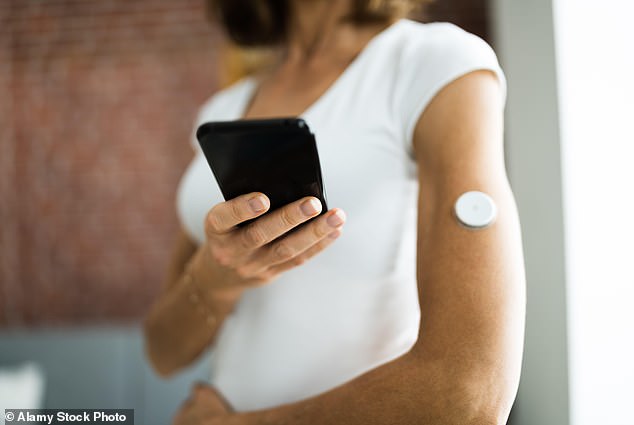
Continuous glucose monitors (CGMs) cost between $50 and $100, and track blood sugar 24/7 for about two weeks at a time

The keto diet emphasizes the role of healthy fats and strictly limits carbohydrates
These devices allowed researchers to measure participants’ glucose levels every five minutes and compare constant levels to the composition of their meals.
‘It really opened our eyes,’ Bills said.
The study, published in January in the journal Frontiers in Neurology, looked at 247 adults with chronic migraine and compared them to 24 healthy controls. As glucose rose, so did migraine prevalence.
The team also separated migraine patients into groups based on their relationship to glucose. Like 50 to 60 percent of participants, Weaver was put into the reactive hypoglycemia group, meaning her glucose would drop within a few hours of eating.

Weaver’s new memoir, Dizzy, explores her journey with chronic migraine
In separate research yet to be published, Bills’s team tested a solution: a ketogenic diet, which strictly limits intake of carbohydrates. Carbs are known to raise glucose. The thought was that preventing spikes in chronic migraine patients would also lower the risk of crashes.
Participants, including Weaver, stuck to a strict keto diet for three months with 15g of carbs allowed per day – the equivalent of a slice of bread, half a cup of cooked pasta or a small piece of fruit.
‘It’s a hard thing to do to your body, and it’s best to be monitored,’ she told the Daily Mail.
For reference, the Dietary Guidelines for Americans recommends 45 to 65 percent of your daily calories should come from carbohydrates. This means someone getting 2,000 calories per day would get 900 to 1,300 calories from carbs, adding up to between 225 and 325g per day.
Bills’s team then worked with each participant to find their individual ‘carb ceiling,’ or the maximum amount they should stick to daily. For Weaver, that’s 50g – about the same as two medium bananas, three medium apples, one cup of cooked white rice, two to three slices of bread or one cup of cooked pasta.
Most patients had a higher carb ceiling, around 80 to 100g, that helped improve their symptoms. ‘We were surprised that it was working so well,’ Bills said.
Weaver is still on the diet, which she said is responsible for drastic improvements in her condition.
‘I have been fine since then,’ she said. ‘I have went from 24/7 debilitating migraines all day, every day for 18 years to like one to three days a month.
‘It’s night and day difference. I got my whole life back.’
Weaver is now down to just two medications for her migraines – an SSRI and an SNRI – along with over-the-counter pain relief as needed. She estimates that, at her worst, she was on nearly a dozen medications.

Bills told the Daily Mail he is excited about the results and publishing data on the keto trial in which Weaver was involved
‘I don’t see myself as like no longer a migraineur,’ she said. ‘I think I’m still very susceptible to all the things, but the response isn’t as intense. Like if I don’t sleep well, then I’m just a little dizzy or a little off, or a little brain fog whereas before, it would just shut me down completely if I didn’t sleep.
‘I think I still I have this migraine brain. It’s just in such a more stable place now.’
Bills cautioned that while the ’emerging data is very exciting,’ a strict diet such as a keto protocol should only be done with a doctor’s supervision. Because migraine is a complex disease, he added, dietary changes are not a ‘silver bullet.’
But wearing a $50 CGM to gather glucose data could provide valuable data for migraine patients to bring to their doctors.
‘It’s very low risk and very inexpensive,’ Bills said. ‘Continuous glucose monitoring is very safe.’
After nearly two decades of dizziness, Weaver is looking forward to making up for lost time, especially with her twin teenagers, as her condition improves.
‘I can work. I can interact with people with an ease that I have not had in all these years,’ she told the Daily Mail.
‘And the bigger thing is that I can be more present with my kids. I don’t have to go to bed at six at night. I don’t have to fight through the dizziness to have conversations with them or to go do something fun. I feel up for doing fun things.
‘It’s a hard experience to put into words, moving from being so debilitatingly ill to feeling pretty fine most of the time.’
Weaver’s memoir, Dizzy, is available now through West Virginia University Press, Amazon and other booksellers nationwide.
First Appeared on
Source link






