Significant Heart Disease Risk Can Be Detected from Routine Mammograms Using AI – Up to 70% Greater
The risk of potentially deadly heart disease can be detected from routine mammograms using AI technology, a new study demonstrated.
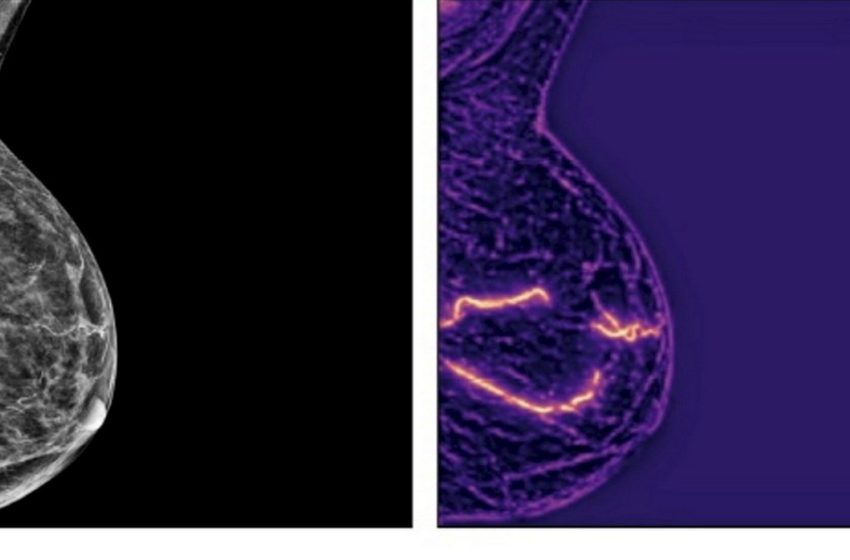
By analyzing the build-up of calcium deposits in the arteries of the breast from standard X-ray mammography scans currently used in breast cancer screening, AI can estimate the risk of heart disease then and later in life.
“Heart disease is the leading cause of death in women worldwide, yet women are consistently underdiagnosed and undertreated compared to men,” said study leader Dr. Hari Trivedi from Emory University in the US. “Mammograms, which women already attend for breast cancer screening, can also reveal calcium deposits in breast arteries and this is linked to heart disease.”
“We wanted to test whether AI could use this to identify women at risk of cardiovascular disease at no extra cost or inconvenience.”
The study, published in the European Heart Journal, included 123,762 women who had taken part in breast screening, but had no known cardiovascular disease.
Researchers used AI to analyze the amount of calcium deposit in the arteries of the breast tissue. Such “arterial calcification” is known to be a sign that the arteries are becoming hardened, and indicates a higher risk of a heart attack or stroke, heart failure, and death.
The amount of arterial calcification in the women’s breast tissue was categorized as severe, moderate, mild, or absent.
The research team then compared these categories with information on whether the women went on to develop serious cardiovascular disease, including a heart attack or stroke.
They found that women with mild calcification were around 30% more likely to suffer serious cardiovascular disease compared to women with no calcification, while those with moderate calcification saw a 70% higher risk.
In women with severe calcification, the risk was 2 to 3-times higher.
“This was true even in younger women under 50, a group often considered low-risk, and held up after accounting for other risk factors like diabetes and smoking,” said Dr. Emory explaining the robustness of the findings.
He said it was the largest study of its kind, and had the added depth of covering multiple ethnicities across the US health service system.
“For women, this means a mammogram you’re already having could also provide important information about your heart health, prompting a conversation with your doctor about preventive steps such as cholesterol testing or medication. For clinicians, it offers a practical way to identify women at cardiovascular risk who are currently being missed.”
“The main steps needed are integrating the AI tool into existing imaging workflows and establishing clear guidelines for notifying patients and doctors, and we are now planning a clinical trial designed to test these steps.”
Professor Lori Daniels, from the University of California San Diego, who wasn’t involved with the study, welcomed the findings.
WOMEN’S HEALTH:
In an accompanying editorial, she said that two-thirds of women aged 50 to 69 in the European Union reported a mammogram within the prior two years, and in the USA, nearly 70% of women aged 45 years and older were up to date with mammography according to American Cancer Society screening guidelines.
At the exact same time, most had no knowledge of their heart disease risk.
AI IN MEDICINE:
“Breast arterial calcification (BAC) has the potential to reframe this mismatch, leveraging a widely adopted cancer-screening platform to identify cardiovascular risk in women who may not otherwise engage with prevention,” wrote Professor Daniels.
“Regardless of the reporting metric ultimately adopted, it is time to shift BAC from observation to implementation, leveraging a touchpoint women already trust, to advance prevention for what remains the leading cause of death among women.”
SHARE This Brilliant Use Of AI In An Underserved Area Of Women’s Medicine…
First Appeared on
Source link






