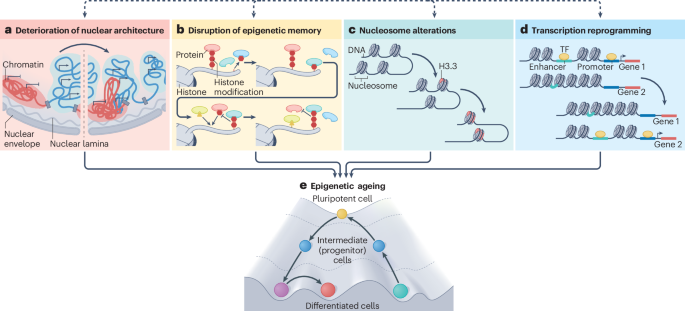
Systemic epigenetic dysregulation as a driver of ageing and a therapeutic target
Guo, J. et al. Aging and aging-related diseases: from molecular mechanisms to interventions and treatments. Signal. Transduct. Target. Ther. 7, 391 (2022).
López-Otín, C., Blasco, M. A., Partridge, L., Serrano, M. & Kroemer, G. Hallmarks of aging: an expanding universe. Cell 186, 243–278 (2023).
Cai, Y. et al. Decoding aging-dependent regenerative decline across tissues at single-cell resolution. Cell Stem Cell 30, 1674–1691 (2023).
da Costa, J. P. et al. A synopsis on aging—theories, mechanisms and future prospects. Ageing Res. Rev. 29, 90–112 (2016).
Lu, Y. R., Tian, X. & Sinclair, D. A. The Information Theory of aging. Nat. Aging 3, 1486–1499 (2023).
Jin, K. Modern biological theories of aging. Aging Dis. 1, 72–74 (2010).
Ferrucci, L., Schrack, J. A., Knuth, N. D. & Simonsick, E. M. Aging and the energetic cost of life. J. Am. Geriatr. Soc. 60, 1768–1769 (2012).
Harman, D. Aging: a theory based on free radical and radiation chemistry. J. Gerontol. 11, 298–300 (1956).
Hayflick, L. & Moorhead, P. S. The serial cultivation of human diploid cell strains. Exp. Cell Res. 25, 585–621 (1961).
Williams, G. C. Pleiotropy, natural selection, and the evolution of senescence. Evolution 11, 398–411 (1957).
Kirkwood, T. B. Evolution of ageing. Nature 270, 301–304 (1977).
Gladyshev, V. N. Aging: progressive decline in fitness due to the rising deleteriome adjusted by genetic, environmental, and stochastic processes. Aging Cell 15, 594–602 (2016).
Wang, K. et al. Epigenetic regulation of aging: implications for interventions of aging and diseases. Signal. Transduct. Target. Ther. 7, 374 (2022).
Yang, J.-H. et al. Loss of epigenetic information as a cause of mammalian aging. Cell 186, 305–326 (2023).
Duffield, T. et al. Epigenetic fidelity in complex biological systems and implications for ageing. Preprint at bioRxiv https://doi.org/10.1101/2023.04.29.538716 (2023).
Issa, J.-P. Aging and epigenetic drift: a vicious cycle. J. Clin. Invest. 124, 24–29 (2014).
Klemm, S. L., Shipony, Z. & Greenleaf, W. J. Chromatin accessibility and the regulatory epigenome. Nat. Rev. Genet. 20, 207–220 (2019).
Bell, C. C., Faulkner, G. J. & Gilan, O. Chromatin-based memory as a self-stabilizing influence on cell identity. Genome Biol. 25, 320 (2024).
Allis, C. D. & Jenuwein, T. The molecular hallmarks of epigenetic control. Nat. Rev. Genet. 17, 487–500 (2016).
Horvath, S. DNA methylation age of human tissues and cell types. Genome Biol. 14, R115 (2013).
Hannum, G. et al. Genome-wide methylation profiles reveal quantitative views of human aging rates. Mol. Cell 49, 359–367 (2013).
Lu, A. T. et al. DNA methylation GrimAge strongly predicts lifespan and healthspan. Aging 11, 303–327 (2019).
Ying, K. et al. Causality-enriched epigenetic age uncouples damage and adaptation. Nat. Aging 4, 231–246 (2024).
Weinberg, D. N. et al. The histone mark H3K36me2 recruits DNMT3A and shapes the intergenic DNA methylation landscape. Nature 573, 281–286 (2019).
Rose, N. R. & Klose, R. J. Understanding the relationship between DNA methylation and histone lysine methylation. Biochim. Biophys. Acta 1839, 1362–1372 (2014).
Espada, J. & Esteller, M. Epigenetic control of nuclear architecture. Cell. Mol. Life Sci. 64, 449–457 (2007).
Sinha, J. et al. The H3.3K36M oncohistone disrupts the establishment of epigenetic memory through loss of DNA methylation. Mol. Cell 84, 3899–3915 (2024).
Rimoldi, M. et al. DNA methylation patterns of transcription factor binding regions characterize their functional and evolutionary contexts. Genome Biol. 25, 146 (2024).
Bielas, J. H. & Loeb, L. A. Quantification of random genomic mutations. Nat. Methods 2, 285–290 (2005).
Gems, D., Virk, R. S. & de Magalhães, J. P. Epigenetic clocks and programmatic aging. Ageing Res. Rev. 101, 102546 (2024).
Meyer, D. H. & Schumacher, B. Aging clocks based on accumulating stochastic variation. Nat. Aging 4, 871–885 (2024).
Tong, H. et al. Quantifying the stochastic component of epigenetic aging. Nat. Aging 4, 886–901 (2024).
Unger Avila, P. et al. Gene regulatory networks in disease and ageing. Nat. Rev. Nephrol. 20, 616–633 (2024).
Liu, Z. et al. Large-scale chromatin reorganization reactivates placenta-specific genes that drive cellular aging. Dev. Cell 57, 1347–1368 (2022).
Tomimatsu, K. et al. Locus-specific induction of gene expression from heterochromatin loci during cellular senescence. Nat. Aging 2, 31–45 (2022).
Su, T.-Y. et al. Aging is associated with functional and molecular changes in distinct hematopoietic stem cell subsets. Nat. Commun. 15, 7966 (2024).
Poscablo, D. M. et al. An age-progressive platelet differentiation path from hematopoietic stem cells causes exacerbated thrombosis. Cell 187, 3090–3107 (2024).
Zhou, S. et al. Age-related intrinsic changes in human bone-marrow-derived mesenchymal stem cells and their differentiation to osteoblasts. Aging Cell 7, 335–343 (2008).
Tarkhov, A. E. et al. Nature of epigenetic aging from a single-cell perspective. Nat. Aging 4, 854–870 (2024).
Gorelov, R. & Hochedlinger, K. A cellular identity crisis? Plasticity changes during aging and rejuvenation. Genes. Dev. 38, 823–842 (2024).
Izgi, H. et al. Inter-tissue convergence of gene expression during ageing suggests age-related loss of tissue and cellular identity. eLife 11, e68048 (2022).
Dos Santos, G. A., Chatsirisupachai, K., Avelar, R. A. & de Magalhães, J. P. Transcriptomic analysis reveals a tissue-specific loss of identity during ageing and cancer. BMC Genomics 24, 644 (2023).
Patrick, R. et al. The activity of early-life gene regulatory elements is hijacked in aging through pervasive AP-1-linked chromatin opening. Cell Metab. 36, 1858–1881 (2024).
Dönertaş, H. M. et al. Gene expression reversal toward pre-adult levels in the aging human brain and age-related loss of cellular identity. Sci. Rep. 7, 5894 (2017).
Iqbal, S. et al. Fetal-like reversion in the regenerating intestine is regulated by mesenchymal asporin. Cell Stem Cell 32, 613–626 (2025).
Chakkalakal, J. V., Jones, K. M., Basson, M. A. & Brack, A. S. The aged niche disrupts muscle stem cell quiescence. Nature 490, 355–360 (2012).
Zhang, L. et al. Modulating mTOR-dependent astrocyte substate transitions to alleviate neurodegeneration. Nat. Aging 5, 468–485 (2025).
Moris, N., Pina, C. & Arias, A. M. Transition states and cell fate decisions in epigenetic landscapes. Nat. Rev. Genet. 17, 693–703 (2016).
Cribbs, D. H. et al. Extensive innate immune gene activation accompanies brain aging, increasing vulnerability to cognitive decline and neurodegeneration: a microarray study. J. Neuroinflammation 9, 179 (2012).
Li, X. et al. Inflammation and aging: signaling pathways and intervention therapies. Signal. Transduct. Target. Ther. 8, 239 (2023).
Holoch, D. et al. A cis-acting mechanism mediates transcriptional memory at Polycomb target genes in mammals. Nat. Genet. 53, 1686–1697 (2021).
Al-Radhawi, M. A., Tripathi, S., Zhang, Y., Sontag, E. D. & Levine, H. Epigenetic factor competition reshapes the EMT landscape. Proc. Natl Acad. Sci. USA 119, e2210844119 (2022).
Basu, A. & Tiwari, V. K. Epigenetic reprogramming of cell identity: lessons from development for regenerative medicine. Clin. Epigenetics 13, 144 (2021).
Crispo, F. et al. Metabolic dysregulations and epigenetics: a bidirectional interplay that drives tumor progression. Cells 8, 798 (2019).
Yücel, A. D. & Gladyshev, V. N. The long and winding road of reprogramming-induced rejuvenation. Nat. Commun. 15, 1941 (2024).
Nichols, M. H. & Corces, V. G. Principles of 3D compartmentalization of the human genome. Cell Rep. 35, 109330 (2021).
Liu, Z., Belmonte, J. C. I., Zhang, W., Qu, J. & Liu, G.-H. Deciphering aging at three-dimensional genomic resolution. Cell Insight 1, 100034 (2022).
Kriukov, D. et al. Nuclear expansion and chromatin structure remodeling in mouse aging neurons. NAR Mol. Med. 1, ugae011 (2024).
Yang, B. A. et al. Three-dimensional chromatin re-organization during muscle stem cell aging. Aging Cell 22, e13789 (2023).
Shaban, H. A. & Gasser, S. M. Dynamic 3D genome reorganization during senescence: defining cell states through chromatin. Cell Death Differ. 32, 9–15 (2025).
Wang, L. et al. Dynamic enhancer interactome promotes senescence and aging. Preprint at bioRxiv https://doi.org/10.1101/2023.05.22.541769 (2023).
Chiang, M. et al. Polymer modeling predicts chromosome reorganization in senescence. Cell Rep. 28, 3212–3223 (2019).
Lee, D. C., Welton, K. L., Smith, E. D. & Kennedy, B. K. A-type nuclear lamins act as transcriptional repressors when targeted to promoters. Exp. Cell Res. 315, 996–1007 (2009).
van Steensel, B. & Belmont, A. S. Lamina-associated domains: links with chromosome architecture, heterochromatin, and gene repression. Cell 169, 780–791 (2017).
Chandra, T. et al. Global reorganization of the nuclear landscape in senescent cells. Cell Rep. 10, 471–483 (2015).
Shah, P. P. et al. An atlas of lamina-associated chromatin across twelve human cell types reveals an intermediate chromatin subtype. Genome Biol. 24, 16 (2023).
Friedman, M. J., Wagner, T., Lee, H., Rosenfeld, M. G. & Oh, S. Enhancer-promoter specificity in gene transcription: molecular mechanisms and disease associations. Exp. Mol. Med. 56, 772–787 (2024).
Chen, H., Li, C., Zhou, Z. & Liang, H. Fast-evolving human-specific neural enhancers are associated with aging-related diseases. Cell Syst. 6, 604–611 (2018).
Del Blanco, B. et al. Kdm1a safeguards the topological boundaries of PRC2-repressed genes and prevents aging-related euchromatinization in neurons. Nat. Commun. 15, 1781 (2024).
Guan, Y. et al. Senescence-activated enhancer landscape orchestrates the senescence-associated secretory phenotype in murine fibroblasts. Nucleic Acids Res. 48, 10909–10923 (2020).
Olan, I. et al. Transcription-dependent cohesin repositioning rewires chromatin loops in cellular senescence. Nat. Commun. 11, 6049 (2020).
Cenni, V. et al. Lamin A involvement in ageing processes. Ageing Res. Rev. 62, 101073 (2020).
Osorio, F. G. et al. Nuclear lamina defects cause ATM-dependent NF-κB activation and link accelerated aging to a systemic inflammatory response. Genes. Dev. 26, 2311–2324 (2012).
Labade, A. S. et al. Expansion in situ genome sequencing links nuclear abnormalities to aberrant chromatin regulation. Science 389, eadt2781 (2025).
de la Rosa, J. et al. Prelamin A causes progeria through cell-extrinsic mechanisms and prevents cancer invasion. Nat. Commun. 4, 2268 (2013).
Alabert, C. et al. Domain model explains propagation dynamics and stability of histone H3K27 and H3K36 methylation landscapes. Cell Rep. 30, 1223–1234 (2020).
Steffen, P. A. & Ringrose, L. What are memories made of? How Polycomb and Trithorax proteins mediate epigenetic memory. Nat. Rev. Mol. Cell Biol. 15, 340–356 (2014).
McCole, R. et al. A conserved switch to less catalytically active Polycomb repressive complexes in non-dividing cells. Cell Rep. 44, 115192 (2025).
Bracken, A. P. et al. The Polycomb group proteins bind throughout the INK4A-ARF locus and are disassociated in senescent cells. Genes. Dev. 21, 525–530 (2007).
von Schimmelmann, M. et al. Polycomb repressive complex 2 (PRC2) silences genes responsible for neurodegeneration. Nat. Neurosci. 19, 1321–1330 (2016).
O’Sullivan, R. J. & Karlseder, J. The great unravelling: chromatin as a modulator of the aging process. Trends Biochem. Sci. 37, 466–476 (2012).
Yang, N. et al. A hyper-quiescent chromatin state formed during aging is reversed by regeneration. Mol. Cell 83, 1659–1676 (2023).
Tvardovskiy, A., Schwämmle, V., Kempf, S. J., Rogowska-Wrzesinska, A. & Jensen, O. N. Accumulation of histone variant H3.3 with age is associated with profound changes in the histone methylation landscape. Nucleic Acids Res. 45, 9272–9289 (2017).
Han, X. & Sun, Z. Epigenetic regulation of KL (klotho) via H3K27me3 (histone 3 lysine [K] 27 trimethylation) in renal tubule cells. Hypertension 75, 1233–1241 (2020).
Sachs, M. et al. Bivalent chromatin marks developmental regulatory genes in the mouse embryonic germline in vivo. Cell Rep. 3, 1777–1784 (2013).
Currey, L. et al. Polycomb repressive complex 2 is critical for mouse cortical glutamatergic neuron development. Cereb. Cortex 34, bhae268 (2024).
He, A. et al. Polycomb repressive complex 2 regulates normal development of the mouse heart. Circ. Res. 110, 406–415 (2012).
Silva-García, C. G. Devo-aging: intersections between development and aging. GeroScience 45, 2145–2159 (2023).
Sen, P. et al. Histone acetyltransferase p300 induces DE Novo super-enhancers to drive cellular senescence. Mol. Cell 73, 684–698 (2019).
Bandyopadhyay, D. & Medrano, E. E. The emerging role of epigenetics in cellular and organismal aging. Exp. Gerontol. 38, 1299–1307 (2003).
Shi, C., Wang, L. & Sen, P. The eroding chromatin landscape of aging stem cells. Transl. Med. Aging 4, 121–131 (2020).
Jung, M. & Pfeifer, G. P. Aging and DNA methylation. BMC Biol. 13, 7 (2015).
Zhang, W., Qu, J., Liu, G.-H. & Belmonte, J. C. I. The ageing epigenome and its rejuvenation. Nat. Rev. Mol. Cell Biol. 21, 137–150 (2020).
Huang, S. Towards a unification of the 2 meanings of ‘epigenetics’. PLoS Biol. 20, e3001944 (2022).
Ler, L. D. et al. Loss of tumor suppressor KDM6A amplifies PRC2-regulated transcriptional repression in bladder cancer and can be targeted through inhibition of EZH2. Sci. Transl. Med. 9, eaai8312 (2017).
Berrozpe, G. et al. Polycomb responds to low levels of transcription. Cell Rep. 20, 785–793 (2017).
Cui, P. et al. Comparative analyses of H3K4 and H3K27 trimethylations between the mouse cerebrum and testis. Genomics Proteomics Bioinformatics 10, 82–93 (2012).
Jadhav, U. et al. Acquired tissue-specific promoter bivalency is a basis for PRC2 necessity in adult cells. Cell 165, 1389–1400 (2016).
Yagi, M. et al. Bivalent chromatin instructs lineage specification during hematopoiesis. Cell 188, 4314–4331.e29 (2025).
Jani, K. S. et al. Histone H3 tail binds a unique sensing pocket in EZH2 to activate the PRC2 methyltransferase. Proc. Natl Acad. Sci. USA 116, 8295–8300 (2019).
Pérez, R. F. et al. A multiomic atlas of the aging hippocampus reveals molecular changes in response to environmental enrichment. Nat. Commun. 15, 5829 (2024).
Zhou, J. X. et al. Combined modulation of polycomb and trithorax genes rejuvenates Î2 cell replication. J. Clin. Invest. 123, 4849–4858 (2013).
Camacho, O. et al. Convergence of aging- and rejuvenation-related epigenetic alterations on PRC2 targets. Mol. Syst. Biol. https://doi.org/10.1038/s44320-026-00195-9 (2026).
Martin, N., Raguz, S., Dharmalingam, G. & Gil, J. Co-regulation of senescence-associated genes by oncogenic homeobox proteins and polycomb repressive complexes. Cell Cycle 12, 2194–2199 (2013).
Chen, H. et al. Polycomb protein Ezh2 regulates pancreatic beta-cell Ink4a/Arf expression and regeneration in diabetes mellitus. Genes Dev. 23, 975–985 (2009).
Farooq, U. et al. An interdependent network of functional enhancers regulates transcription and EZH2 loading at the INK4a/ARF locus. Cell Rep. 34, 108898 (2021).
Bruggeman, S. W. M. et al. Ink4a and Arf differentially affect cell proliferation and neural stem cell self-renewal in Bmi1-deficient mice. Genes Dev. 19, 1438–1443 (2005).
Schwörer, S. et al. Epigenetic stress responses induce muscle stem-cell ageing by Hoxa9 developmental signals. Nature 540, 428–432 (2016).
Leclerc, K. et al. Hox genes are crucial regulators of periosteal stem cell identity. Development 150, dev201391 (2023).
de Lima Camillo, L. P., Asif, M. H., Horvath, S., Larschan, E. & Singh, R. Histone mark age of human tissues and cell types. Sci. Adv. 11, eadk9373 (2025).
Yoshioka, K. et al. Hoxa10 mediates positional memory to govern stem cell function in adult skeletal muscle. Sci. Adv. 7, eabd7924 (2021).
Kurosu, H. et al. Suppression of aging in mice by the hormone Klotho. Science 309, 1829–1833 (2005).
Castner, S. A. et al. Longevity factor klotho enhances cognition in aged nonhuman primates. Nat. Aging 3, 931–937 (2023).
Wang, Q., Sun, J., Wang, R. & Sun, J. Inhibition of EZH2 mitigates peritoneal fibrosis and lipid precipitation in peritoneal mesothelial cells mediated by klotho. Ren. Fail. 45, 2149411 (2023).
Lu, T. T.-H. et al. The Polycomb-dependent epigenome controls β cell dysfunction, dedifferentiation, and diabetes. Cell Metab. 27, 1294–1308 (2018).
Maze, I. et al. Critical role of histone turnover in neuronal transcription and plasticity. Neuron 87, 77–94 (2015).
Saade, E., Pirozhkova, I., Aimbetov, R., Lipinski, M. & Ogryzko, V. Molecular turnover, the H3.3 dilemma and organismal aging (hypothesis). Aging Cell 14, 322–333 (2015).
Guo, R. et al. BS69/ZMYND11 reads and connects histone H3.3 lysine 36 trimethylation-decorated chromatin to regulated pre-mRNA processing. Mol. Cell 56, 298–310 (2014).
Wen, H. et al. ZMYND11 links histone H3.3K36me3 to transcription elongation and tumour suppression. Nature 508, 263–268 (2014).
Trovato, M. et al. Histone H3.3 lysine 9 and 27 control repressive chromatin at cryptic enhancers and bivalent promoters. Nat. Commun. 15, 7557 (2024).
Kori, Y. et al. Multi-omic profiling of histone variant H3.3 lysine 27 methylation reveals a distinct role from canonical H3 in stem cell differentiation. Mol. Omics 18, 296–314 (2022).
Masuzawa, R., Rosa Flete, H. K., Shimizu, J. & Kawano, F. Age-related histone H3.3 accumulation associates with a repressive chromatin in mouse tibialis anterior muscle. J. Physiol. Sci. 74, 41 (2024).
Harada, A. et al. Incorporation of histone H3.1 suppresses the lineage potential of skeletal muscle. Nucleic Acids Res. 43, 775–786 (2015).
Tsurumi, A. & Li, W. X. Global heterochromatin loss: a unifying theory of aging? Epigenetics 7, 680–688 (2012).
Lemus, A. J. J. et al. The interplay of epigenetic remodelling and transposon-mediated genomic instability in ageing and longevity. Open Biol. 16, 250093 (2026).
Dubey, S. K. et al. Histone deficiency and hypoacetylation in the aging retinal pigment epithelium. Aging Cell 23, e14108 (2024).
Liu, L. et al. Chromatin modifications as determinants of muscle stem cell quiescence and chronological aging. Cell Rep. 4, 189–204 (2013).
Lin, C. et al. Arginine hypomethylation-mediated proteasomal degradation of histone H4-an early biomarker of cellular senescence. Cell Death Differ. 27, 2697–2709 (2020).
Ivanov, A. et al. Lysosome-mediated processing of chromatin in senescence. J. Cell Biol. 202, 129–143 (2013).
Hu, Y. et al. Multiscale footprints reveal the organization of cis-regulatory elements. Nature 638, 779–786 (2025).
Ding, M. et al. Integration of ATAC-Seq and RNA-Seq reveals FOSL2 drives human liver progenitor-like cell aging by regulating inflammatory factors. BMC Genomics 24, 260 (2023).
Yu, X., Wang, Y., Song, Y., Gao, X. & Deng, H. AP-1 is a regulatory transcription factor of inflammaging in the murine kidney and liver. Aging Cell 22, e13858 (2023).
Karakaslar, E. O. et al. Transcriptional activation of Jun and Fos members of the AP-1 complex is a conserved signature of immune aging that contributes to inflammaging. Aging Cell 22, e13792 (2023).
Martínez-Zamudio, R. I. et al. AP-1 imprints a reversible transcriptional programme of senescent cells. Nat. Cell Biol. 22, 842–855 (2020).
Ferreira, F. J. et al. FOXM1 expression reverts aging chromatin profiles through repression of the senescence-associated pioneer factor AP-1. Nat. Commun. 16, 2931 (2025).
Ribeiro, R. et al. In vivo cyclic induction of the FOXM1 transcription factor delays natural and progeroid aging phenotypes and extends healthspan. Nat. Aging 2, 397–411 (2022).
Byrns, C. N., Saikumar, J. & Bonini, N. M. Glial AP1 is activated with aging and accelerated by traumatic brain injury. Nat. Aging 1, 585–597 (2021).
Markov, G. J. et al. AP-1 is a temporally regulated dual gatekeeper of reprogramming to pluripotency. Proc. Natl Acad. Sci. USA 118, e2104841118 (2021).
Liu, Y. et al. AP-1 activity is a major barrier of human somatic cell reprogramming. Cell. Mol. Life Sci. 78, 5847–5863 (2021).
Rubin, H. Ordered heterogeneity and its decline in cancer and aging. Adv. Cancer Res. 98, 117–147 (2007).
Bozukova, M. et al. Aging is associated with increased chromatin accessibility and reduced polymerase pausing in liver. Mol. Syst. Biol. 18, e11002 (2022).
Gadek, M. et al. Aging activates escape of the silent X chromosome in the female mouse hippocampus. Sci. Adv. 11, eads8169 (2025).
Liesenfelder, S. et al. Epigenetic editing at individual age-associated CpGs affects the genome-wide epigenetic aging landscape. Nat. Aging 5, 997–1009 (2025).
Moqri, M. et al. PRC2-AgeIndex as a universal biomarker of aging and rejuvenation. Nat. Commun. 15, 5956 (2024).
Mitchell, W. et al. Multi-omics characterization of partial chemical reprogramming reveals evidence of cell rejuvenation. eLife 12, RP90579 (2024).
Murphy, M. P. & Partridge, L. Toward a control theory analysis of aging. Annu. Rev. Biochem. 77, 777–798 (2008).
Sun, E. D., Michaels, T. C. T. & Mahadevan, L. Optimal control of aging in complex networks. Proc. Natl Acad. Sci. USA 117, 20404–20410 (2020).
Cookis, T., Lydecker, A., Sauer, P., Kasinath, V. & Nogales, E. Structural basis for the inhibition of PRC2 by active transcription histone posttranslational modifications. Nat. Struct. Mol. Biol. 32, 393–404 (2025).
Namitz, K. E. W., Tan, S. & Cosgrove, M. S. Hierarchical assembly of the MLL1 core complex regulates H3K4 methylation and is dependent on temperature and component concentration. J. Biol. Chem. 299, 102874 (2023).
Tibben, B. M. & Rothbart, S. B. Mechanisms of DNA methylation regulatory function and crosstalk with histone lysine methylation. J. Mol. Biol. 436, 168394 (2024).
Sengstack, J. et al. Systematic identification of single transcription factor perturbations that drive cellular and tissue rejuvenation. Proc. Natl Acad. Sci. USA 123, e2515183123 (2026).
Johnstone, S. E. et al. Large-scale topological changes restrain malignant progression in colorectal cancer. Cell 182, 1474–1489 (2020).
Chu, L. et al. Induction of senescence-associated secretory phenotype underlies the therapeutic efficacy of PRC2 inhibition in cancer. Cell Death Dis. 13, 155 (2022).
Yu, W. et al. The PRC2 complex epigenetically silences GATA4 to suppress cellular senescence and promote the progression of breast cancer. Transl. Oncol. 46, 102014 (2024).
Shaulian, E. AP-1-The Jun proteins: oncogenes or tumor suppressors in disguise? Cell. Signal. 22, 894–899 (2010).
First Appeared on
Source link






