
Two compounds found in surprising substance reverse liver disease damage, study suggests
Two organic compounds in the cannabis plant may be the key to reversing fatty liver disease, a silent killer that affects at least a quarter of Americans.
Metabolic dysfunction-associated steatotic liver disease (MASLD) is the most common chronic liver disorder in the world, driven by obesity, poor response to insulin, high blood pressure and high cholesterol.
Researchers in Israel believe that CBD (cannabidiol) and CBG (cannabigerol), the non-psychoactive chemicals in the cannabis plant that have been studied for years for their medicinal properties, can reverse liver damage that causes chronic MASLD.
Both federally legal in the US, CBD is commonly used for stress relief, anxiety, pain management and sleep support, while CBG is often marketed for inflammation, mental clarity, and digestive issues. Both are available in tinctures, topicals and edibles, though evidence for many of these uses remains largely anecdotal or preclinical.
To test the substances’ effects on liver health, the researchers injected obese mice with either compound or a placebo drug.
The compounds did not work as researchers expected. Rather than acting through classical cannabinoid receptors, the typical targets of cannabis-related compounds, CBD and CBG, appeared to reprogram liver metabolism, prompting the organ to rely on an alternative energy-buffering system.
Treated mice showed a notable increase in phosphocreatine, a molecule that acts as a rapid energy reserve for cells, alongside enhanced activity of lysosomes, which act as the cell’s cleanup and recycling centers.
This combination helped the liver better manage the toxic buildup of fat and reduced markers of inflammation and insulin resistance, all without changes to diet or physical activity.
Metabolic dysfunction-associated steatotic liver disease (MASLD) is the world’s most common chronic liver disorder, driven by obesity, insulin resistance, high blood pressure and high cholesterol (stock)
The beneficial effects were not limited to the liver.
Mice receiving either CBD or CBG also showed whole-body improvements, including lower cholesterol levels and reduced fat mass. These changes occurred despite the mice maintaining their Western-style high-fat diets, suggesting those compounds make the liver more resilient to excess fat and energy dysregulation.
To test the effects of CBD and CBG on fatty liver disease, researchers at the Hebrew University of Jerusalem fed male mice either a standard diet or a high-fat diet for 14 weeks to make them obese and metabolically unhealthy, mimicking the conditions that contribute to MASLD in humans.
After this period, the mice were divided into three injectable treatment groups: CBD, CBG or a placebo, which they would receive for four weeks, all while continuing their high-fat diet.
For the first three weeks in the CBD group, researchers administered five milligrams per kilogram of body weight, then increased the dosage to 10 mg for the final week.
CBG followed a similar pattern, starting at 12.5mg and escalating to 25mg.
Researchers monitored body weight, body composition and glucose tolerance throughout the treatment period.
When four weeks were up, researchers collected liver tissue, blood, and other samples to analyze fat accumulation, cholesterol levels, the expression of genes, and cellular metabolism, or the way cells use and store energy.

Researchers in Israel believe that CBD and CBG, non-psychoactive cannabis compounds with a long history of medicinal study, may reverse the liver damage underlying MASLD (stock)
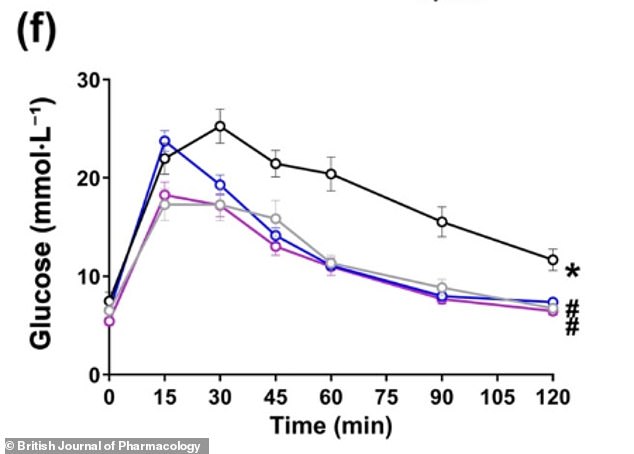
Mice treated with CBD (blue) or CBG (purple) cleared glucose from the bloodstream more efficiently than untreated HFD-fed mice (black and gray)
Mice given CBD and CBG, having gained fat on an unhealthy diet for a month, saw both a reduction in fat mass and a boost in lean mass, signaling that the compounds fundamentally altered how the body stores and uses energy.
Mice treated with the cannabinoids also showed normal fasting glucose levels, which had been elevated on their high-fat diets.
To get a clearer picture of how the mice were processing sugar, the researchers calculated a standard measure of insulin resistance called HOMA-IR.
Mice fed the high-fat diet had a sharp rise in this score, meaning their bodies had stopped responding properly to insulin.
Treatment with CBG brought this number down significantly, while CBD also helped, though to a slightly lesser degree.
When the researchers looked at blood fats, they found that high-fat diet mice had modestly elevated triglycerides, a common type of fat in the blood. Both CBD and CBG lowered those levels.
The effect was even more striking with total cholesterol and LDL cholesterol, the so-called ‘bad’ cholesterol. Both were markedly higher in the high-fat diet group, and treatment with either compound brought them down, with CBG leading to the biggest improvement.
Inside the liver, the compounds activate an energy sensor called AMPK, which restores energy balance by switching the cell from consuming energy to producing it. Activated at times of low energy or fasting, this metabolic switch boosts glucose uptake and fat burning.
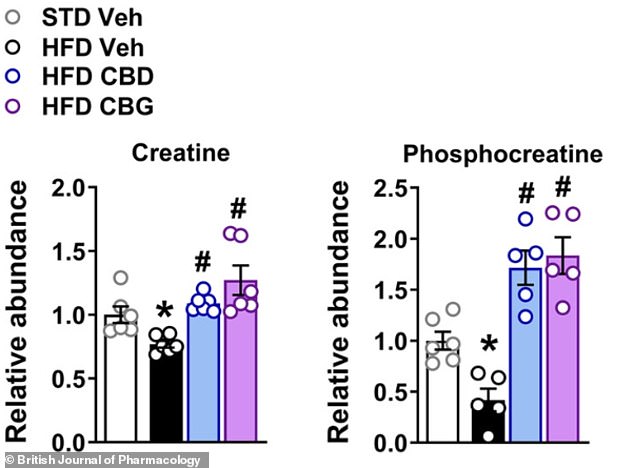
The figures show the levels of creatine and phosphocreatine, which together form an energy-buffering system. STD Veh is healthy diet + placebo; HFD Veh is high-fat diet + placebo; HFD CBD is high-fat diet + CBD treatment; HFD CBG is high-fat diet + CBG treatment. Both CBD and CBG restored and even increased the liver’s energy reserves, suggesting those livers had a much greater capacity to handle energy stress
But in this case, the mice did not show the usual increased fat-burning or energy-producing pathways.
Instead, researchers found that the livers of the treated mice had built up high levels of creatine and phosphocreatine, which act as back-up batteries for cells, storing and releasing energy when needed.
This system is more commonly seen in muscles. The liver does not normally rely on it. But under treatment with CBD and CBG, the liver ramped up its creatine energy-buffering system, essentially giving itself a new way to manage energy stress brought on by obesity and a high-fat diet.
To determine how the compounds were affecting the liver on a molecular level, researchers carried out a comprehensive analysis of all fats, or lipids, present in liver tissue.
The results, published in the British Journal of Clinical Pharmacology, showed that the compounds did not simply reduce the amount of fat; they fundamentally altered the composition of liver lipids.
Triglycerides—the primary component of fatty liver—accounted for nearly half of all lipids that decreased following treatment. Ceramides, a class of fats associated with insulin resistance and metabolic inflammation, were also lowered.
At the same time, the compounds increased levels of several phospholipids, including a specialized group called lysobisphosphatidic acids (LBPAs).
These lipids are concentrated in lysosomes, the cellular compartments responsible for breaking down and recycling fats. The rise in LBPAs corresponded with improved lysosomal function, suggesting enhanced clearance of harmful fats.
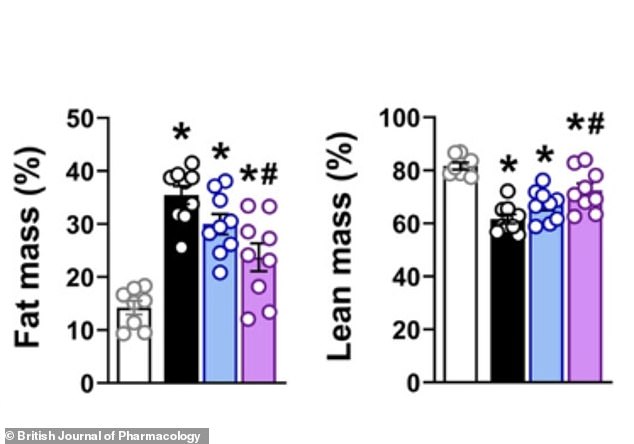
The figures show that mice treated with CBD and CBG lost fat mass and gained lean mass, showing the compounds shifted how the body stores and uses energy even on a high-fat diet
Whether these results hold up in human subjects remains to be seen. Still, the findings carry some notable implications. It uncovered a previously unrecognized means for reducing metabolic stress on the liver that could be targeted with drugs.
If similar pathways exist in humans, compounds like CBD and CBG may offer a new approach to treating MASLD, previously known as non-alcoholic fatty liver disease.
Between 80 million and 100 million Americans have MASLD, some without knowing it.
For most, the condition remains silent, causing no noticeable symptoms. But for others, it can progress to metabolic dysfunction-associated steatohepatitis (MASH), a more severe form marked by inflammation and scarring.
Over time, MASH can lead to cirrhosis, liver failure and hepatocellular carcinoma — a type of liver cancer.
With obesity and diabetes rates continuing to climb, the number of people affected is expected to grow, underscoring the urgent need for effective treatments. The current treatment protocol focuses on addressing the underlying metabolic drivers, including obesity, insulin resistance and high cholesterol.
‘Despite the increasing clinical burden of MASLD, no pharmacological treatments have been approved to date,’ the study authors write.
‘This therapeutic gap underscores the urgent need for novel pharmacological agents that can target the underlying mechanisms of disease progression.’
The results were promising, but the researchers caution that the CBD and CBG compounds used in their experiment were precisely calibrated for the mice — doses and purity levels that do not necessarily translate to products on store shelves.
Commercial formulations vary widely in concentration, purity and bioavailability, and none have been tested in human clinical trials for fatty liver disease.
First Appeared on
Source link






