A measles outbreak in Florida is simmering, but we know almost nothing about it. We went to investigate
Ave Maria, Florida
—
One Wednesday this month, loud cries erupted from two teenage girls huddled over a cellphone in the parking lot of a local supermarket. They had just learned that a classmate at the private K-12 school just a few blocks north had been diagnosed with measles. Unvaccinated students were going to be kept out of school for the next month.
I overheard the commotion just as I was packing my notebook away and preparing to leave Ave Maria, a small but rapidly growing planned community on the northwestern edge of the Florida Everglades. It’s a place with little formal leadership aside from the real estate developers and the heads of the Catholic Church that the community is based around.
I was visiting because one of the largest measles outbreaks the United States has seen on a college campus in decades erupted just a few blocks west at Ave Maria University at the end of January, but very little information was being shared with the public.
I tried to get in touch with the Florida Department of Health and Ave Maria University over phone and email for a month, with no response, before making a trip to the center of the outbreak. There have now been more than 100 cases reported in the county: 88 confirmed and 16 probable.
My visit had shown me that a lot was happening outside of the public view, but that night at the grocery store, I was feeling defeated. I still couldn’t pin down the trajectory of the outbreak or gauge the level of risk to the community.
Just a couple hours earlier, the university president had reprimanded me for stopping by a town hall he was hosting for students, and he refused to answer my questions about the outbreak. Visits to county health department offices had yielded new phone numbers to call but no new calls back. And for the previous two days, many local folks had met my questions about measles with a certain level of indifference and some past-tense reflections, as if the outbreak were long over.
There was a general sense among the public that the outbreak had died down and that the broader community had been spared. Yes, there was a measles outbreak, but it had stayed “across the street,” as the locals say, referencing a small road that serves as an unofficial border between the university campus and the rest of the town.
But for a small group of in-the-know people — including local health care providers and a former assistant secretary of the US Department of Health and Human Services who call the town home — this moment in the supermarket parking lot was anxiously anticipated: Measles had jumped from the university to the broader town. A second wave of the outbreak was probably underway.
Measles is extraordinarily contagious. Florida’s outbreak hasn’t reached the record-breaking scale of others the US has seen over the past year, such those in Texas and South Carolina, but it is still unusual; before last year, there were only 10 other times in the two and a half decades since the US declared measles eliminated that an outbreak had surpassed 50 cases. Vaccines can effectively prevent it, but any place where the vaccination rate has dropped below about 95% is at risk.
Ave Maria sits near the middle of Collier County, in the southwest part of the state, which has reported at least 104 measles cases since the start of January, and more than 10% of them have come in the past two weeks, since measles made the jump “across the street.” Most cases in the county have been concentrated among the 15-to-24 age group — which aligns with an outbreak on the university campus — but not all cases have been among college students. A growing share are among young children and teens.
The handful of community leaders I was able to connect with had positive things to say about the way the Florida health department is managing the response to the measles outbreak. But the department has not responded to any of the calls or emails I’ve sent over the past month, so I have no firsthand accounts of the work it has done or what it’s still doing.
Experts in infectious disease and in public health say that the unusual lack of public communication has probably hindered the public health response. More could have been done to get out ahead of the spread and prevent more cases.
“Most jurisdictions do what they can to get the word out about measles outbreaks because they need the public’s partnership and engagement to bring the outbreak under control,” said Dr. Caitlin Rivers, an epidemiologist and director of the Center for Outbreak Response Innovation at the Johns Hopkins Bloomberg School of Public Health.
“Because measles is airborne and very transmissible, there are sometimes public exposures like at the grocery store or medical clinic that need broader attention,” she said.
Ave Maria brands itself as “a big kind of small town,” and it’s quickly getting bigger. Thousands of newly constructed homes rise in the middle of a rural part of Collier County roughly halfway between Naples to the west and Fort Lauderdale to the east, and acres of flat land stand ready to house thousands more. About 8,000 people live in Ave Maria, and about 1,300 students are enrolled at the university.
I traveled into town along a highway dubbed Alligator Alley, and after a few miles along a rural road with signs warning drivers about panther crossings, palm trees sprung up to line the last few miles to the town center. A massive Catholic church dominates the main square, ringed by shops and restaurants, and it directly faces the Ave Maria University campus.
As I stood in the center of it all, a bright spot under my feet caught my eye: A Domino’s Pizza logo had been emblazoned on one of the pavement stones; the pizza chain’s former CEO had also founded Ave Maria University and helped build the town around it.
People riding golf carts, bikes and scooters seemed to outnumber those in cars as they zipped around the town center. Most were dressed in typical Florida attire: casual sundresses and polo shirts. I noticed one golf cart driver who stood out for being dressed in a sharp navy blue suit and colorful pocket square — and I would quickly learn what it means to visit a small town.
I walked a few blocks for a meeting I had scheduled with Tony Musingo, a local physician assistant who had diagnosed many of the community’s first measles cases. He didn’t want to meet in his office; the clinic had moved its check-in desk outside when the measles outbreak started a few weeks earlier and was generally limiting who could go inside as a precaution.
A graduate student studying theology at the university — who also happened to be one of the early measles cases on campus — helped coordinate my meeting with Musingo. He brought us upstairs, through an office and out to a patio for a shaded place to sit and talk. The well-dressed man in a suit who I had seen in the golf cart was waiting to greet us: Michael Caputo, an assistant HHS secretary for public affairs in the first Trump administration during the first year of the Covid-19 pandemic.
Caputo now runs a startup biotech business from the small Florida town and studies theology at the university. His company makes a device that works as a smoke detector for airborne viruses, and the university is using pilot versions of it in some of its classrooms.
As measles cases grow nationwide, other states with outbreaks have sent out timely status updates and regularly made leaders available for questions. The South Carolina health department started hosting weekly media briefings when there were less than a dozen cases associated with their local outbreak. Utah state health officials have also held multiple briefings offering updates on the situation there.
South Carolina, Utah and many other states with far fewer cases than Florida — which currently ranks third for the most measles cases in 2026, according to data from the US Centers for Disease Control and Prevention — have stood up measles dashboards that provide details about case demographics and exposure locations. Florida provides a case count by county and an option to filter by age group, but there’s no context provided. It updates once a week.
Age group data from the Florida health department suggests that the outbreak has spread beyond the college campus, said Rivers, the Johns Hopkins epidemiologist whose organization developed a measles case tracker and worked with health departments from across the country to help them learn from their experiences responding to measles.
This “goes to show that outbreak information is usually of interest to the entire community,” she said.
Ave Maria University had a “campus health update” alert on its website that was updated regularly in the early days of the outbreak, often with more recent case counts than the state health department was sharing. But at some point, updates slowed, and the university started linking back to the state health department data — essentially revising the case count down from what it had reported earlier.
The university prominently identifies a contact for media inquiries on the website, but that person did not reply to any of my questions about the outbreak. During my visit, she sent me an email to reiterate the university president’s message that I was not welcome on campus but also did not return my phone call after that.
In Ave Maria, the public health response to the measles outbreak seemed to be as elusive as the Florida panther: prominent in the area but largely hidden from public view. You need to know the right places to look.
The lack of official communication from the public health department has left unofficial town leaders to fill gaps in awareness and guidance — and they’re all seemingly coordinated by Caputo.
When I couldn’t get in touch with the state health department or the university, I tried other ways to learn more about the measles outbreak in Ave Maria: I reached out to the local parish, builders associations, community organizations and more.
Most didn’t respond to me, but they had all told Caputo about my calls. This is a small town. He knew I was coming and exactly who I was trying to talk to.

The role may not be one Caputo asked for, but it’s one that he seems to have embraced. He says he’s coordinated with the local parish on a message about measles that has been shared at multiple masses and helped draft the email communication that the K-12 school sent out once a student tested positive.
A few weeks ago, email and text blasts sent from his company — Ave Maria Biotech — informed thousands of residents about a webinar that local health care providers would be hosting about the measles outbreak with Dr. Robert Redfield, director of the CDC during the first Trump administration who is now chief science adviser for Ave Maria Biotech.
In it, Redfield warned about a second wave and raised specific concerns about the risk that measles poses to pregnant women.
He also encouraged vaccination. He spent a significant portion of time sharing negative reflections on Covid-era policies but was staunch in his support of the measles-mumps-rubella (MMR) vaccine — especially because the Catholic Church has formally dispelled concerns about the use of fetal tissue in development, endorsing vaccination as not only morally permissible but virtuous.
When I asked Caputo how he views his own role in the current measles response, he said he’s just a concerned resident.
“Nobody wants a self-proclaimed expert coming in to tell you what to do, so I tried to keep myself out of it,” he said. “I think the community has done a great job.”
Caputo and Musingo, the local physician assistant, agree that when they heard about the first cases of the outbreak, they thought things would be much worse than they have been.
Congregation is a key part of life in Ave Maria, they said. Strong community ties bring people together at daily church services, for neighborhood rosary walks, for university classes and community events. They worried that there were too many opportunities for the virus to spread.
“The students really did their part,” Caputo said, saying that they isolated when sick and generally stayed on campus and away from town. “The people here look out for each other.”
Still, as a resident, Caputo says, he would have liked to hear more from the state health department.
“This is a storytelling town, and they’re missing the narrative,” he said.
In many ways, it seems that Florida leadership is particularly focused on avoiding the narrative. But history has shown that public communication is critical to help families and health care providers do their part during a measles outbreak.
It’s important for families to hear directly from the department of health during a measles outbreak because they’re the experts, said Dr. Jennifer Takagishi, vice president of the Florida chapter of the American Academy of Pediatrics. The department is central to the data gathering and to the response.
“For families who may or may not have access to a physician or other provider, they are the safety net for all these families, too,” she said. “There’s a lot more scientific and medicine hesitancy and mistrust than there used to be, so being able to really give doctors the tools to be able to explain the data in a meaningful and up-to-date way is also very important.”
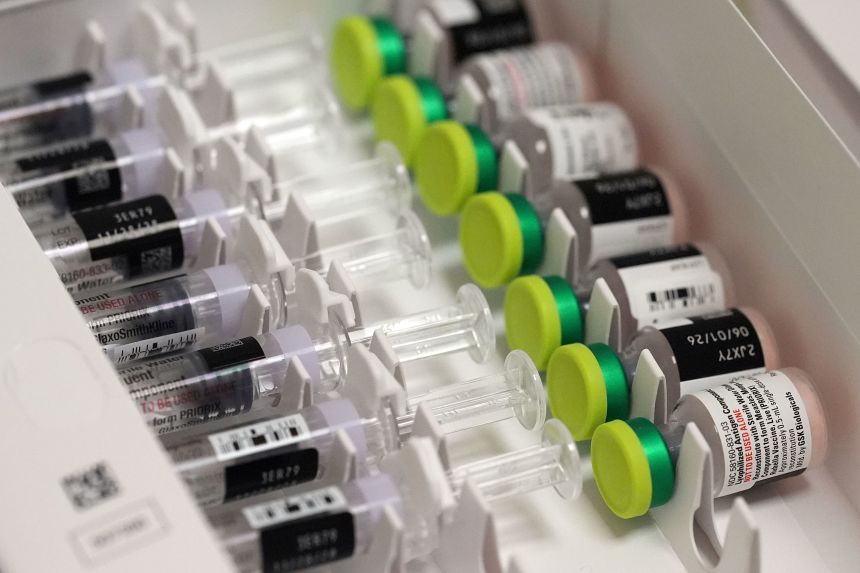
There are also suspicions among local health care providers that even though the public health department was able to host a vaccination clinic, it couldn’t advertise about the value of the vaccine or that it was available — and that made it less successful than it could have been. This is a point I would have liked to clarify with the state health department, if I was able to connect with them.
What I do know is that Florida Surgeon General Dr. Joseph Ladapo has spoken at events supporting the “medical freedom” movement. He wants to ban mRNA vaccines in Florida and announced plans to end childhood vaccination mandates in the state, likening them to slavery.
“I do know that some of our state officials are vaccine hesitant themselves, and are therefore not promoting vaccines for our families,” said Takagishi, who practices a few hours north of Ave Maria, in Tampa. “What we’d really prefer is that they’re out in front of the public in advance, so that they can be encouraging families to get vaccinated, to get information, so that we can avoid the outbreaks or manage them very early and not wait until there’s a significant number of people before we act.”

The lack of official narrative may have led local folks to a premature sense of safety, believing that the outbreak had ended even as cases continue to add up.
“Oh, yeah, that’s over” was a common refrain during my first few laps around town. But some doubt would creep in, and they’d follow up to be sure: “Isn’t it?”
Ave Maria University’s “campus health update” link has been removed from the university’s homepage. The last update from a couple weeks ago reads that “there are currently zero nurse-assessed confirmed cases on campus” — but it shows a total case count that is nearly a dozen cases behind the current total for the county.
A measles case at the K-12 school seems to have piqued the public’s doubt and shifted perceptions at least a bit, though. Only after the revelation of cases among a younger student did I hear any mention of fear.
Jessica Tolentino doesn’t live in Ave Maria, but her family is in town often; her husband oversees some of the new development there, and her teenage son has friends at the private K-12 school.
Earlier that week, her son told her that a few of his friends were meeting up to play basketball in Ave Maria but that he didn’t want to go because “something was going around.” It was very unlike him, she said, so she was already on alert when the measles news landed.
“And if the case was just confirmed Wednesday, that means it’s been spreading around long before,” Tolentino said.
She’s especially nervous because her younger son has a heart condition that makes him more susceptible to severe complications from a viral infection. He had to avoid certain vaccines for the first seven years of his life, she said. And although he’s vaccinated against measles now, his weakened immune system puts him at higher risk.
“We might have to avoid town for a while,” she said.
Caputo and Musingo are still hopeful. They say all signs indicate that the second wave will be small. But even after spending time in town and visiting the nearest health department, I still don’t know what the formal public health response will look like.
The Diocese of Venice in Florida, a jurisdiction of the Catholic Church that runs the K-12 school in Ave Maria, says it has consulted with the Florida health department to develop its quarantine protocol for students. The school has also cancelled some events for parents amid the outbreak.
The diocese mentioned that a local pediatrician in Ave Maria was offering MMR vaccination through extended hours at her office and local house visits. It said the Florida health department has made itself available to answer questions about measles and the situation – responding to hourly phone calls early on — but didn’t say anything about whether it might help with promoting vaccination or managing the outbreak on the ground.
I ran into one dad who was visiting the pediatrician with two of his five kids. He was quick to say it was for a regular checkup, not for measles. The family had just moved to town over the summer, and a few kids were old enough to attend school.
Keeping unvaccinated kids out of school is a “tough decision,” he said. “But it’s safe and decisive and will hopefully help get things under control.”
Hearing about the measles case at the school made him “a little nervous,” he said, “but we’re vaccinated.”
Time will tell how the measles outbreak will progress in Ave Maria, but I’ll keep watching the weekly case count and trying to get more information from the Florida health department.
First Appeared on
Source link






