
A Snake Parasite Never Seen in Humans Was Found Living Inside a Woman’s Brain After Months of Lung Damage and Memory Loss
For 12 months, physicians treated a 64-year-old Australian woman for a lung condition of unknown origin. They administered steroids, then immunosuppressants, then monoclonal antibodies. Her symptoms improved temporarily but never resolved completely. When she developed memory problems and depression in mid-2022, doctors ordered a brain scan. The image showed a single lesion in the right frontal lobe. During open surgery to examine the tissue, they found a live, bright red worm.
Canberra Health Services reported on August 11 2023 the first documented human infection with Ophidascaris robertsi, a parasitic roundworm native to Australian carpet pythons. The 80mm third-stage larva removed from the patient’s brain represented a pathogen never before seen in humans.
The case, published in the US Centers for Disease Control and Prevention’s Emerging Infectious Diseases journal, described an infection that migrated through multiple organs before reaching the central nervous system. According to the CDC case report on Ophidascaris robertsi infection, this is the first known instance of the parasite invading a human host.
From Abdominal Pain to Brain Surgery
The patient, from southeastern New South Wales, first presented to a local hospital in late January 2021 with three weeks of abdominal pain and diarrhea, followed by dry cough and night sweats. Blood tests showed a peripheral blood eosinophil count of 9.8 × 10⁹ cells per liter, approximately 20 times the reference range upper limit.
A CT scan revealed multifocal pulmonary opacities with surrounding ground-glass changes, a finding that Medical News Today defines as increased density in lung tissue that can indicate inflammation or infection. The scan also showed lesions on the liver and spleen. Bronchoalveolar lavage returned 30 percent eosinophils with no detectable pathogens.
Physicians diagnosed eosinophilic pneumonia of unclear etiology and prescribed prednisolone 25mg daily. The patient improved partially but returned three weeks later with recurrent fever and persistent cough while still on the medication. CT scans showed persistent hepatic and splenic lesions plus migratory pulmonary opacities. Lung biopsy confirmed eosinophilic pneumonia. Bacterial, fungal and mycobacterial cultures were negative. Serologic testing for Echinococcus, Fasciola and Schistosoma returned no antibodies. Fecal examinations showed no parasites.
Researchers detected a monoclonal T-cell receptor gene rearrangement suggesting T-cell driven hypereosinophilic syndrome. Treatment began with prednisolone 50mg daily and mycophenolate 1g twice daily. Given the patient’s travel history to regions with endemic parasites two to three decades earlier, physicians administered ivermectin 200µg/kg orally for two consecutive days with a repeat dose after 14 days.
CT imaging in mid-2021 showed improvement in pulmonary and hepatic lesions but unchanged splenic lesions. In January 2022, physicians added mepolizumab 300mg every four weeks because prednisolone could not be reduced below 20mg daily without respiratory symptom flare.
Worm Discovered in Frontal Lobe Lesion
Over three months in 2022, the patient developed forgetfulness and worsening depression while continuing immunosuppressive therapy. Brain MRI showed a 13 × 10mm peripherally enhancing right frontal lobe lesion.
In June 2022, surgeons performed an open biopsy. They observed a stringlike structure within the lesion and removed a live, motile helminth measuring 80mm long and 1mm in diameter. Tissue histopathology showed a benign organizing inflammatory cavity with prominent eosinophilia.
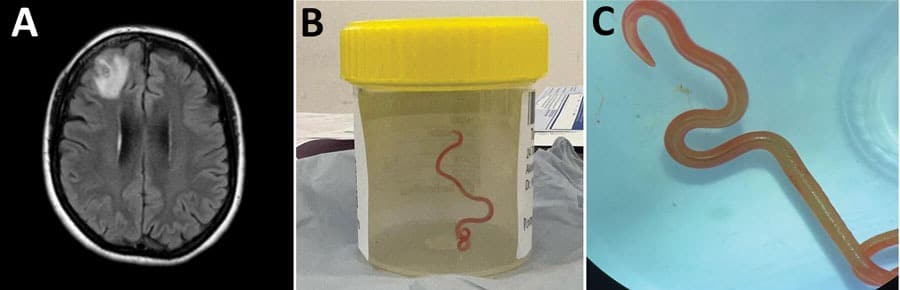
The team provisionally identified the helminth as a third-stage larva of Ophidascaris robertsi based on its distinctive red color, three active ascaridoid-like lips, presence of a cecum and absence of a fully developed reproductive system.
Independent PCR-based sequencing at the University of Sydney and the University of Melbourne both returned more than 99.7 percent sequence match to Ophidascaris robertsi isolates, confirming the peer-reviewed findings published in Emerging Infectious Diseases.
Python Parasite’s Unusual Life Cycle
Ophidascaris robertsi nematodes are endemic to Australia, with carpet pythons (Morelia spilota) as definitive hosts. Adult nematodes inhabit the python’s esophagus and stomach, shedding eggs in the snake’s feces. Small mammals ingest the eggs, and larvae migrate to thoracic and abdominal organs. The life cycle completes when pythons consume infected intermediate hosts. No human infection with any Ophidascaris species had been reported previously.
The patient resided near a lake area inhabited by carpet pythons. Although she reported no direct snake contact, she regularly collected native vegetation, warrigal greens (Tetragonia tetragonioides), from around the lake for cooking. Investigators hypothesized that she inadvertently consumed Ophidascaris robertsi eggs either directly from contaminated vegetation or indirectly through contaminated hands or kitchen equipment.
The clinical and radiologic progression indicated a dynamic process of larval migration to multiple organs accompanied by eosinophilia in blood and tissues, consistent with visceral larva migrans syndrome. Ophidascaris larvae survive for extended periods in animal hosts. Laboratory rats have remained infected with third-stage larvae for more than four years. The patient’s immunosuppression may have enabled the larvae to migrate into the central nervous system, an invasion not previously reported with Ophidascaris species.
Treatment and Recovery
Following surgical removal of the larva, the patient received ivermectin 200µg/kg daily for two days and albendazole 400mg twice daily for four weeks to address potential larvae in other organs. Dexamethasone was administered in a weaning course starting at 4mg twice daily over 10 weeks, with all other immunosuppression discontinued.
Six months after surgery and three months after ceasing dexamethasone, the patient’s peripheral blood eosinophil count remained within reference range. Neuropsychiatric symptoms had improved but persisted. CT imaging showed resolution of pulmonary and hepatic lesions.
No further human infections with Ophidascaris robertsi have been documented since this case.
First Appeared on
Source link






