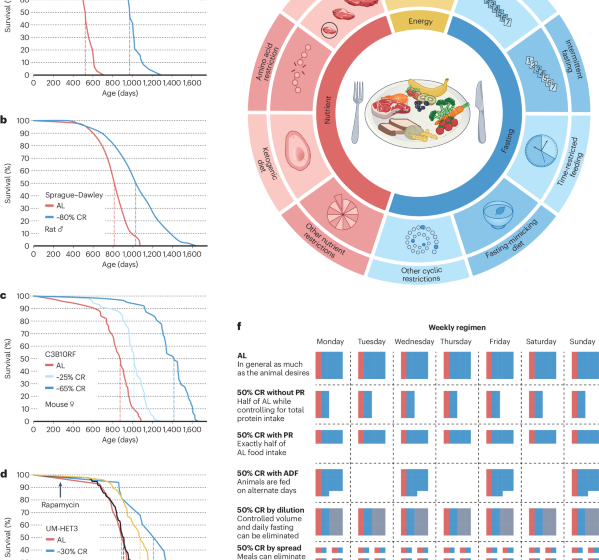
Dietary restriction in aging and longevity
Weindruch, R. & Walford, R. L. Dietary restriction in mice beginning at 1 year of age: effect on life-span and spontaneous cancer incidence. Science 215, 1415–1418 (1982).
Goodrick, C. L., Ingram, D. K., Reynolds, M. A., Freeman, J. R. & Cider, N. L. Differential effects of intermittent feeding and voluntary exercise on body weight and lifespan in adult rats. J. Gerontol. 38, 36–45 (1983).
Yu, B. P., Masoro, E. J. & McMahan, C. A. Nutritional influences on aging of Fischer 344 rats: I. Physical, metabolic, and longevity characteristics. J. Gerontol. 40, 657–670 (1985).
Beauchene, R. E., Bales, C. W., Bragg, C. S., Hawkins, S. T. & Mason, R. L. Effect of age of initiation of feed restriction on growth, body composition, and longevity of rats. J. Gerontol. 41, 13–19 (1986).
Goodrick, C. L., Ingram, D. K., Reynolds, M. A., Freeman, J. R. & Cider, N. L. Effects of intermittent feeding upon growth and life span in rats. Gerontology 28, 233–241 (1982).
Ross, M. H. Length of life and nutrition in the rat. J. Nutr. 75, 197–210 (1961).
Harrison, D. E. & Archer, J. R. Genetic differences in effects of food restriction on aging in mice. J. Nutr. 117, 376–382 (1987).
Weindruch, R., Walford, R. L., Fligiel, S. & Guthrie, D. The retardation of aging in mice by dietary restriction: longevity, cancer, immunity and lifetime energy intake. J. Nutr. 116, 641–654 (1986).
Bartke, A. et al. Extending the lifespan of long-lived mice. Nature 414, 412–412 (2001).
Flurkey, K., Astle, C. M. & Harrison, D. E. Life extension by diet restriction and N-acetyl-L-cysteine in genetically heterogeneous mice. J. Gerontol. A Biol. Sci. Med. Sci. 65, 1275–1284 (2010).
Miller, R. A. et al. Rapamycin, but not resveratrol or simvastatin, extends life span of genetically heterogeneous mice. J. Gerontol. A Biol. Sci. Med. Sci. 66, 191–201 (2011).
Kealy, R. D. et al. Effects of diet restriction on life span and age-related changes in dogs. J. Am. Vet. Med. Assoc. 220, 1315–1320 (2002).
Pinney, D. O., Stephens, D. F. & Pope, L. S. Lifetime effects of winter supplemental feed level and age at first parturition on range beef cows. J. Anim. Sci. 34, 1067–1074 (1972).
Comfort, A. The effect of age on growth-resumption in fish (Lebistes) checked by food restriction. Gerontologia 4, 177–186 (1960).
Austad, S. N. Life extension by dietary restriction in the bowl and doily spider, Frontinella pyramitela. Exp. Gerontol. 24, 83–92 (1989).
Chmilar, S. L. et al. Caloric restriction extends lifespan in a clonal plant. Ecol. Lett. 27, e14444 (2024).
Minina, E. A. et al. Autophagy mediates caloric restriction-induced lifespan extension in Arabidopsis. Aging Cell 12, 327–329 (2013).
Turturro, A. et al. Growth curves and survival characteristics of the animals used in the biomarkers of aging program. J. Gerontol. A Biol. Sci. Med. Sci. 54, B492–B501 (1999).
Swindell, W. R. Dietary restriction in rats and mice: a meta-analysis and review of the evidence for genotype-dependent effects on lifespan. Ageing Res. Rev. 11, 254–270 (2012).
Brown-Borg, H. M., Borg, K. E., Meliska, C. J. & Bartke, A. Dwarf mice and the ageing process. Nature 384, 33–33 (1996).
Bartke, A. & Brown-Borg, H. Life extension in the dwarf mouse. Curr. Top. Dev. Biol. 63, 189–225 (2004).
Mattison, J. A. et al. Studies of aging in ames dwarf mice: effects of caloric restriction. J. Am. Aging Assoc. 23, 9–16 (2000).
Sun, L. Y. et al. Growth hormone-releasing hormone disruption extends lifespan and regulates response to caloric restriction in mice. eLife 2, e01098 (2013).
Arum, O., Bonkowski, M. S., Rocha, J. S. & Bartke, A. The growth hormone receptor gene-disrupted mouse fails to respond to an intermittent fasting diet. Aging Cell 8, 756–760 (2009).
Bonkowski, M. S., Rocha, J. S., Masternak, M. M., Regaiey, K. A. A. & Bartke, A. Targeted disruption of growth hormone receptor interferes with the beneficial actions of calorie restriction. Proc. Natl Acad. Sci. USA 103, 7901–7905 (2006).
Smolen, A., Smolen, T. N. & van de Kamp, J. L. Sensitivity of inbred and selectively bred mice to ethanol. Alcohol 4, 57–62 (1987).
Liao, C., Rikke, B. A., Johnson, T. E., Diaz, V. & Nelson, J. F. Genetic variation in the murine lifespan response to dietary restriction: from life extension to life shortening. Aging Cell 9, 92–95 (2010).
Mattson, M. P. Genes and behavior interact to determine mortality in mice when food is scarce and competition fierce. Aging Cell 9, 448–449 (2010).
Ikeno, Y. et al. Housing density does not influence the longevity effect of calorie restriction. J. Gerontol. A Biol. Sci. Med. Sci. 60, 1510–1517 (2005).
Liao, C., Rikke, B. A., Johnson, T. E., Diaz, V. & Nelson, J. F. No evidence that competition for food underlies lifespan shortening by dietary restriction in multiply housed mice: response to commentary. Aging Cell 9, 450–452 (2010).
Rikke, B. A., Liao, C. -Y., McQueen, M. B., Nelson, J. F. & Johnson, T. E. Genetic dissection of dietary restriction in mice supports the metabolic efficiency model of life extension. Exp. Gerontol. 45, 691–701 (2010).
Speakman, J. R. & Mitchell, S. E. Caloric restriction. Mol. Aspects Med. 32, 159–221 (2011).
Senior, A. M. Estimating genetic variance in life-span response to diet: insights from statistical simulation. J. Gerontol. A Biol. Sci. Med. Sci. 78, 392–396 (2022).
Unnikrishnan, A. et al. Reevaluation of the effect of dietary restriction on different recombinant inbred lines of male and female mice. Aging Cell 20, e13500 (2021).
Francesco, A. D. et al. Dietary restriction impacts health and lifespan of genetically diverse mice. Nature https://doi.org/10.1038/s41586-024-08026-3 (2024).
Shenhar, B. et al. Heritability of intrinsic human life span is about 50% when confounding factors are addressed. Science 391, 504–510 (2026).
Kapahi, P., Kaeberlein, M. & Hansen, M. Dietary restriction and lifespan: lessons from invertebrate models. Ageing Res. Rev. 39, 3–14 (2017).
Carey, J. R. et al. Life history response of Mediterranean fruit flies to dietary restriction. Aging Cell 1, 140–148 (2002).
Carey, J. R. et al. Food pulses increase longevity and induce cyclical egg production in Mediterranean fruit flies. Funct. Ecol. 16, 313–325 (2002).
Carey, J. R. et al. Stochastic dietary restriction using a Markov-chain feeding protocol elicits complex, life history response in medflies. Aging Cell 4, 31–39 (2005).
Fanson, B. G., Weldon, C. W., Pérez-Staples, D., Simpson, S. J. & Taylor, P. W. Nutrients, not caloric restriction, extend lifespan in Queensland fruit flies (Bactrocera tryoni). Aging Cell 8, 514–523 (2009).
Hansen, B. C., Ortmeyer, H. K. & Bodkin, N. L. Prevention of obesity in middle-aged monkeys: food intake during body weight clamp. Obes. Res. 3, 199s–204s (1995).
Bodkin, N. L., Alexander, T. M., Ortmeyer, H. K., Johnson, E. & Hansen, B. C. Mortality and morbidity in laboratory-maintained rhesus monkeys and effects of long-term dietary restriction. J. Gerontol. A Biol. Sci. Med. Sci. 58, B212–B219 (2003).
Lane, M. A., Mattison, J. A., Roth, G. S., Brant, L. J. & Ingram, D. K. Effects of long-term diet restriction on aging and longevity in primates remain uncertain. J. Gerontol. A Biol. Sci. Med. Sci. 59, B405–B407 (2004).
Ingram, D. K. et al. Dietary restriction and aging: the initiation of a primate study. J. Gerontol. 45, B148–B163 (1990).
Lane, M. A. et al. Calorie restriction lowers body temperature in rhesus monkeys, consistent with a postulated anti-aging mechanism in rodents. Proc. Natl Acad. Sci. USA 93, 4159–4164 (1996).
Lane, M. A., Mattison, J., Ingram, D. K. & Roth, G. S. Caloric restriction and aging in primates: relevance to humans and possible CR mimetics. Microsc. Res. Tech. 59, 335–338 (2002).
Mattison, J. A. et al. Impact of caloric restriction on health and survival in rhesus monkeys from the NIA study. Nature 489, 318–321 (2012).
Colman, R. J. et al. Caloric restriction delays disease onset and mortality in rhesus monkeys. Science 325, 201–204 (2009).
Mattison, J. A. et al. Caloric restriction improves health and survival of rhesus monkeys. Nat. Commun. 8, 14063 (2017).
Mitchell, S. J. et al. Daily fasting improves health and survival in male mice independent of diet composition and calories. Cell Metab 29, 221–228 (2019).
Stayer-Wilburn, O. et al. Dysregulation of astrocytic Aquaporin-1 in the brains of oldest-old rhesus macaques: the NIA caloric restriction study. GeroScience 47, 781–793 (2025).
Weindruch, R. et al. Measures of body size and growth in rhesus and squirrel monkeys subjected to long-term dietary restriction. Am. J. Primatol. 35, 207–228 (1995).
Stuart, J. A. & Page, M. M. Plasma IGF-1 is negatively correlated with body mass in a comparison of 36 mammalian species. Mech. Ageing Dev. 131, 591–598 (2010).
Pifferi, F. et al. Caloric restriction increases lifespan but affects brain integrity in grey mouse lemur primates. Commun. Biol. 1, 30 (2018).
Pifferi, F. et al. Promoting healthspan and lifespan with caloric restriction in primates. Commun. Biol. 2, 107 (2019).
Carlson, A. J. & Hoelzel, F. Apparent prolongation of the life span of rats by intermittent fasting one figure. J. Nutr. 31, 363–375 (1946).
Pietrocola, F. et al. Metabolic effects of fasting on human and mouse blood in vivo. Autophagy 13, 567–578 (2017).
The CALERIE Research Group. Final Protocol for the Phase 2 Study, version 1.5 (The CALERIE Research Group, 2009).
Most, J., Tosti, V., Redman, L. M. & Fontana, L. Calorie restriction in humans: an update. Ageing Res. Rev. 39, 36–45 (2017).
Stewart, T. M. et al. Comprehensive assessment of long-term effects of reducing intake of energy phase 2 (CALERIE Phase 2) screening and recruitment: methods and results. Contemp. Clin. Trials 34, 10–20 (2013).
Ravussin, E. et al. A 2-year randomized controlled trial of human caloric restriction: feasibility and effects on predictors of health span and longevity. J. Gerontol. A Biol. Sci. Med. Sci. 70, 1097–1104 (2015).
Shen, W. et al. Effect of 2-year caloric restriction on organ and tissue size in nonobese 21- to 50-year-old adults in a randomized clinical trial: the CALERIE study. Am. J. Clin. Nutr. 114, 1295–1303 (2021).
Kraus, W. E. et al. 2 years of calorie restriction and cardiometabolic risk (CALERIE): exploratory outcomes of a multicentre, phase 2, randomised controlled trial. Lancet Diabetes Endocrinol. 7, 673–683 (2019).
Waziry, R. et al. Effect of long-term caloric restriction on DNA methylation measures of biological aging in healthy adults from the CALERIE trial. Nat Aging 3, 248–257 (2023).
McCay, C. M. in Cowdry’s Problems of Ageing (ed. Lansing, A. I.) 139–202 (The Williams & Wilkins Company, 1952).
Weindruch, R. H., Kristie, J. A., Cheney, K. E. & Walford, R. L. Influence of controlled dietary restriction on immunologic function and aging. Fed. Proc. 38, 2007–2016 (1979).
Sun, L., Akha, A. A. S., Miller, R. A. & Harper, J. M. Life-span extension in mice by preweaning food restriction and by methionine restriction in middle age. J. Gerontol. A Biol. Sci. Med. Sci. 64A, 711–722 (2009).
Dhahbi, J. M., Kim, H. -J., Mote, P. L., Beaver, R. J. & Spindler, S. R. Temporal linkage between the phenotypic and genomic responses to caloric restriction. Proc. Natl Acad. Sci. USA 101, 5524–5529 (2004).
Forster, M. J., Morris, P. & Sohal, R. S. Genotype and age influence the effect of caloric intake on mortality in mice. FASEB J. 17, 690–692 (2003).
Lipman, R. D., Smith, D. E., Bronson, R. T. & Blumberg, J. Is late-life caloric restriction beneficial? Aging Clin. Exp. Res. 7, 136–139 (1995).
Lipman, R. D., Smith, D. E., Blumberg, J. B. & Bronson, R. T. Effects of caloric restriction or augmentation in adult rats: longevity and lesion biomarkers of aging. Aging Clin. Exp. Res. 10, 463–470 (1998).
Hahn, O. et al. A nutritional memory effect counteracts the benefits of dietary restriction in old mice. Nat. Metab. 1, 1059–1073 (2019).
Senior, A. M. et al. Dietary macronutrient content, age-specific mortality and lifespan. Proc. Biol. Sci. 286, 20190393 (2019).
Mitchell, S. J. et al. Effects of sex, strain, and energy intake on hallmarks of aging in mice. Cell Metab. 23, 1093–1112 (2016).
Richardson, A., Austad, S. N., Ikeno, Y., Unnikrishnan, A. & McCarter, R. J. Significant life extension by ten percent dietary restriction. Ann. N. Y. Acad. Sci. 1363, 11–17 (2016).
Everitt, A. V., Porter, B. D. & Wyndham, J. R. Effects of caloric intake and dietary composition on the development of proteinuria, age-associated renal disease and longevity in the male rat. Gerontology 28, 168–175 (1982).
Cherkin, A. Letter to editor. Age 2, 51–51 (1979).
Cutler, R. G. in Testing the Theories of Aging (eds. Adelman, R. C. et al.) 25–114 (CRC Press, 1982).
Hayflick, L. How and Why We Age? (Random House, 1994).
Berry, R. J., Jakobson, M. E. & Triggs, G. S. Survival in wild-living mice. Mammal Rev. 3, 46–57 (1973).
Weindruch, R. & Walford, R. L. The Retardation of Aging and Disease by Dietary Restriction (C. C. Thomas, 1988).
Austad, S. N. Does caloric restriction in the laboratory simply prevent overfeeding and return house mice to their natural level of food intake? Sci. Aging Knowledge Environ. 2001, pe3 (2001).
Austad, S. N. & Kristan, D. M. Are mice calorically restricted in nature?. Aging Cell 2, 201–207 (2003).
Masoro, E. J. in Calorie Restriction, Aging and Longevity (eds. Everitt, A. V. et al.) 3–14 (Springer, 2010).
Wolf, A. M. Rodent diet aids and the fallacy of caloric restriction. Mech. Ageing Dev. 200, 111584 (2021).
Bertrand, H. A., Lynd, F. T., Masoro, E. J. & Yu, B. P. Changes in adipose mass and cellularity through the adult life of rats fed ad libitum or a life-prolonging restricted diet. J. Gerontol. 35, 827–835 (1980).
Solon-Biet, S. M. et al. The ratio of macronutrients, not caloric intake, dictates cardiometabolic health, aging, and longevity in ad libitum-fed mice. Cell Metab. 19, 418–430 (2014).
Lane, P. W. & Dickie, M. M. The effect of restricted food intake on the life span of genetically obese mice. J. Nutr. 64, 549–554 (1958).
Harrison, D. E., Archer, J. R. & Astle, C. M. Effects of food restriction on aging: separation of food intake and adiposity. Proc. Natl Acad. Sci. USA 81, 1835–1838 (1984).
Ahima, R. S. Adipose tissue as an endocrine organ. Obesity 14, 242S–249S (2006).
Funcke, J. -B. & Scherer, P. E. Beyond adiponectin and leptin: adipose tissue-derived mediators of inter-organ communication. J. Lipid Res. 60, 1648–1697 (2019).
Rubner, M. Das Problem der Lebensdauer und Seine Beziehungen zu Wachstum und Ernährung (Druck und Verlag von R. Oldenbourg, 1908).
Pearl, R. The Rate of Living (Univ. London Press, 1928).
Sacher, G. A. in Handbook of The Biology of Aging (eds. Finch, C. E. et al.) 582–638 (Litton Educational Publishing, 1977).
Masoro, E. J., Yu, B. P. & Bertrand, H. A. Action of food restriction in delaying the aging process. Proc. Natl Acad. Sci. USA 79, 4239–4241 (1982).
Will, L. C. & McCay, C. M. Ageing, basal metabolism, and retarded growth. Arch. Biochem. 481, 485 (1943).
McCarter, R., Masoro, E. J. & Yu, B. P. Does food restriction retard aging by reducing the metabolic rate?. Am. J. Physiol. Endocrinol. Metab. 248, E488–E490 (1985).
McCarter, R. J. & McGee, J. R. Transient reduction of metabolic rate by food restriction. Am. J. Physiol. Endocrinol. Metab. 257, E175–E179 (1989).
McCarter, R. J. & Palmer, J. Energy metabolism and aging: a lifelong study of Fischer 344 rats. Am. J. Physiol. Endocrinol. Metab. 263, E448–E452 (1992).
McCarter, R. J. M. et al. Physical activity as a factor in the action of dietary restriction on aging: effects in Fischer 344 rats. Aging Clin. Exp. Res. 9, 73–79 (1997).
Finch, C. E. Longevity, Senescence, and The Genome (The University of Chicago Press, 1990).
Guarente, L. & Picard, F. Calorie restriction—the SIR2 connection. Cell 120, 473–482 (2005).
Sohal, R. S., Ferguson, M., Sohal, B. H. & Forster, M. J. Life span extension in mice by food restriction depends on an energy imbalance. J. Nutr. 139, 533–539 (2009).
Masoro, E. J. Overview of calorie restriction and aging. In Calorie Restriction Society Conference III, vol. 2 (DVD set) (Calorie Restriction Society, 2004).
Mitchell, S. E. et al. The effects of graded levels of calorie restriction: VIII. impact of short term calorie and protein restriction on basal metabolic rate in the C57BL/6 mouse. Oncotarget 8, 17453–17474 (2017).
Banks, A. S. et al. A consensus guide to preclinical indirect calorimetry experiments. Nat. Metab. 7, 1765–1780 (2025).
Keil, G., Cummings, E. & de Magalhães, J. P. Being cool: how body temperature influences ageing and longevity. Biogerontology 16, 383–397 (2015).
Conti, B. & Cabo, R. de. Promoting health and survival through lowered body temperature. Nat. Aging https://doi.org/10.1038/s43587-025-00850-0 (2025).
Walford, R. L. & Liu, R. K. Husbandry, life span, and growth rate of the annual fish, Cynolebias adloffi. Exp. Gerontol. 1, 161–168 (1965).
Liu, R. K. & Walford, R. L. Increased growth and life-span with lowered ambient temperature in the annual fish, Cynolebias adloffi. Nature 212, 1277–1278 (1966).
Klass, M. R. Aging in the nematode Caenorhabditis elegans: major biological and environmental factors influencing life span. Mech. Ageing Dev. 6, 413–429 (1977).
Miquel, J., Lundgren, P. R., Bensch, K. G. & Atlan, H. Effects of temperature on the life span, vitality and fine structure of Drosophila melanogaster. Mech. Ageing Dev. 5, 347–370 (1976).
Rikke, B. A. & Johnson, T. E. Lower body temperature as a potential mechanism of life extension in homeotherms. Exp. Gerontol. 39, 927–930 (2004).
Duffy, P. H. et al. Effect of chronic caloric restriction on physiological variables related to energy metabolism in the male Fischer 344 rat. Mech. Ageing Dev. 48, 117–133 (1989).
Rikke, B. A. et al. Strain variation in the response of body temperature to dietary restriction. Mech. Ageing Dev. 124, 663–678 (2003).
Mitchell, S. E. et al. The effects of graded levels of calorie restriction: III. Impact of short term calorie and protein restriction on mean daily body temperature and torpor use in the C57BL/6 mouse. Oncotarget 6, 18314–18337 (2015).
Soare, A., Cangemi, R., Omodei, D., Holloszy, J. O. & Fontana, L. Long-term calorie restriction, but not endurance exercise, lowers core body temperature in humans. Aging 3, 374–379 (2011).
Zhao, Z. et al. Body temperature is a more important modulator of lifespan than metabolic rate in two small mammals. Nat. Metab. 4, 320–326 (2022).
Conti, B. et al. Transgenic mice with a reduced core body temperature have an increased life span. Science 314, 825–828 (2006).
Walford, R. L. & Spindler, S. R. The response to calorie restriction in mammals shows features also common to hibernation: a cross-adaptation hypothesis. J. Gerontol. A Biol. Sci. Med. Sci. 52A, B179–B183 (1997).
Hambly, C., Mercer, J. G. & Speakman, J. R. Hunger Does not diminish over time in mice under protracted caloric restriction. Rejuvenation Res. 10, 533–542 (2007).
Derous, D. et al. The effects of graded levels of calorie restriction: VI. Impact of short-term graded calorie restriction on transcriptomic responses of the hypothalamic hunger and circadian signaling pathways. Aging 8, 642–661 (2016).
Minor, R. K. et al. The arcuate nucleus and neuropeptide Y contribute to the antitumorigenic effect of calorie restriction. Aging Cell 10, 483–492 (2011).
Chiba, T. et al. A key role for neuropeptide Y in lifespan extension and cancer suppression via dietary restriction. Sci. Rep. 4, 4517 (2014).
Duffy, P. H., Feuers, R., Nakamura, K. D., Leakey, J. & Hart, R. W. Effect of chronic caloric restriction on the synchronization of various physiological measures in old female Fischer 344 rats. Chronobiol. Int. 7, 113–124 (1990).
Acosta-Rodríguez, V. A., de Groot, M. H. M., Rijo-Ferreira, F., Green, C. B. & Takahashi, J. S. Mice under caloric restriction self-impose a temporal restriction of food intake as revealed by an automated feeder system. Cell Metab. 26, 267–277 (2017).
Nelson, W. & Halberg, F. Meal-timing, circadian rhythms and life span of mice. J. Nutr. 116, 2244–2253 (1986).
Masoro, E. J., Shimokawa, I., Higami, Y., McMahan, C. A. & Yu, B. P. Temporal pattern of food intake not a factor in the retardation of aging processes by dietary restriction. J. Gerontol. A Biol. Sci. Med. Sci. 50A, B48–B53 (1995).
Pak, H. H. et al. Fasting drives the metabolic, molecular and geroprotective effects of a calorie-restricted diet in mice. Nat Metab. 3, 1327–1341 (2021).
Acosta-Rodríguez, V. et al. Circadian alignment of early onset caloric restriction promotes longevity in male C57BL/6J mice. Science 376, 1192–1202 (2022).
Liu, X. et al. Calorie restriction and calorie dilution have different impacts on body fat, metabolism, behavior, and hypothalamic gene expression. Cell Rep. 39, 110835 (2022).
Anson, R. M. et al. Intermittent fasting dissociates beneficial effects of dietary restriction on glucose metabolism and neuronal resistance to injury from calorie intake. Proc. Natl Acad. Sci. USA 100, 6216–6220 (2003).
Hatori, M. et al. Time-restricted feeding without reducing caloric intake prevents metabolic diseases in mice fed a high-fat diet. Cell Metab. 15, 848–860 (2012).
Calabrese, E. J. & Mattson, M. P. The catabolic – anabolic cycling hormesis model of health and resilience. Ageing Res. Rev. 102, 102588 (2024).
Marosi, K. et al. 3-Hydroxybutyrate regulates energy metabolism and induces BDNF expression in cerebral cortical neurons. J. Neurochem. 139, 769–781 (2016).
Youm, Y. -H. et al. The ketone metabolite β-hydroxybutyrate blocks NLRP3 inflammasome–mediated inflammatory disease. Nat. Med. 21, 263–269 (2015).
Shimazu, T. et al. Suppression of oxidative stress by β-hydroxybutyrate, an endogenous histone deacetylase inhibitor. Science 339, 211–214 (2013).
Mattson, M. P. The cyclic metabolic switching theory of intermittent fasting. Nat. Metab. 7, 665–678 (2025).
Nelson, W. & Halberg, F. Schedule-shifts, circadian rhythms and lifespan of freely-feeding and meal-fed mice. Physiol. Behav. 38, 781–788 (1986).
Nelson, W. Food restriction, circadian disorder and longevity of rats and mice. J. Nutr. 118, 284–289 (1988).
Tognini, P. et al. Distinct circadian signatures in liver and gut clocks revealed by ketogenic diet. Cell Metab. 26, 523–538 (2017).
Longo, V. D. & Panda, S. Fasting, circadian rhythms, and time-restricted feeding in healthy lifespan. Cell Metab. 23, 1048–1059 (2016).
Zhang, S.-Q. et al. NR1D1 inhibition enhances autophagy and mitophagy in Alzheimer’s disease models. Aging Dis. https://doi.org/10.14336/ad.2024.1654 (2025).
Segall, P. E. & Timiras, P. S. Patho-physiologic findings after chronic tryptophan deficiency in rats: a model for delayed growth and aging. Mech. Ageing Dev. 5, 109–124 (1976).
Orentreich, N., Matias, J. R., DeFelice, A. & Zimmerman, J. A. Low methionine ingestion by rats extends life span. J. Nutr. 123, 269–274 (1993).
Miller, R. A. et al. Methionine-deficient diet extends mouse lifespan, slows immune and lens aging, alters glucose, T4, IGF-I and insulin levels, and increases hepatocyte MIF levels and stress resistance. Aging Cell 4, 119–125 (2005).
Masoro, E. J. et al. Dietary modulation of the progression of nephropathy in aging rats: an evaluation of the importance of protein. Am. J. Clin. Nutr. 49, 1217–1227 (1989).
Green, C. L., Lamming, D. W. & Fontana, L. Molecular mechanisms of dietary restriction promoting health and longevity. Nat. Rev. Mol. Cell Biol. 23, 56–73 (2022).
Green, C. L. et al. Dietary restriction of isoleucine increases healthspan and lifespan of genetically heterogeneous mice. Cell Metab. 35, 1976–1995 (2023).
Yeh, C. -Y. et al. Late-life protein or isoleucine restriction impacts physiological and molecular signatures of aging. Nat. Aging 4, 1760–1771 (2024).
Miller, R. A. et al. Glycine supplementation extends lifespan of male and female mice. Aging Cell 18, e12953 (2019).
Piper, M. D. W. et al. Matching dietary amino acid balance to the in silico-translated exome optimizes growth and reproduction without cost to lifespan. Cell Metab. 25, 610–621 (2017).
Lane, M. A., Ingram, D. K. & Roth, G. S. 2-deoxy-D-glucose feeding in rats mimics physiologic effects of calorie restriction. J. Anti Aging Med. 1, 327–337 (1998).
Lane, M. A., Ingram, D. K. & Roth, G. S. The serious search for an anti-aging pill. Sci. Am. 287, 36–41 (2002).
Ingram, D. K. & Roth, G. S. Calorie restriction mimetics: can you have your cake and eat it, too? Ageing Res. Rev. 20, 46–62 (2015).
Pistell, P. J. et al. An avocado extract enriched in mannoheptulose prevents the negative effects of a high-fat diet in mice. Nutrients 14, 155 (2021).
Ingram, D. K. et al. Characterization and mechanisms of action of avocado extract enriched in mannoheptulose as a candidate calorie restriction mimetic. J. Agric. Food Chem. 69, 7367–7376 (2021).
Simcox, J. & Lamming, D. W. The central moTOR of metabolism. Dev. Cell 57, 691–706 (2022).
Moore, T. et al. Dietary energy balance modulates signaling through the Akt/mammalian target of rapamycin pathways in multiple epithelial tissues. Cancer Prev. Res. 1, 65–76 (2008).
Sharma, N., Castorena, C. M. & Cartee, G. D. Tissue-specific responses of IGF-1/insulin and mTOR signaling in calorie restricted rats. PLoS ONE 7, e38835 (2012).
Tulsian, R., Velingkaar, N. & Kondratov, R. Caloric restriction effects on liver mTOR signaling are time-of-day dependent. Aging 10, 1640–1648 (2018).
Ham, D. J. et al. Distinct and additive effects of calorie restriction and rapamycin in aging skeletal muscle. Nat. Commun. 13, 2025 (2022).
Unnikrishnan, A., Kurup, K., Salmon, A. B. & Richardson, A. Is rapamycin a dietary restriction mimetic?. J. Gerontol. A Biol. Sci. Med. Sci. 75, glz060 (2019).
Sharp, Z. D. & Strong, R. The role of mTOR signaling in controlling mammalian life span: what a fungicide teaches us about longevity. J. Gerontol. A Biol. Sci. Med. Sci. 65, 580–589 (2010).
Harrison, D. E. et al. Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature 460, 392–395 (2009).
Miller, R. A. et al. Rapamycin-mediated lifespan increase in mice is dose and sex dependent and metabolically distinct from dietary restriction. Aging Cell 13, 468–477 (2014).
Inagaki, T. et al. Endocrine regulation of the fasting response by PPARα-mediated induction of fibroblast growth factor 21. Cell Metab. 5, 415–425 (2007).
Fazeli, P. K. et al. FGF21 and the late adaptive response to starvation in humans. J. Clin. Invest. 125, 4601–4611 (2015).
Laeger, T. et al. FGF21 is an endocrine signal of protein restriction. J. Clin. Invest. 124, 3913–3922 (2014).
Phillips, E. J. & Simons, M. J. P. Rapamycin not dietary restriction improves resilience against pathogens: a meta-analysis. GeroScience 45, 1263–1270 (2023).
Ivimey-Cook, E. R., Sultanova, Z. & Maklakov, A. A. Rapamycin, not metformin, mirrors dietary restriction-driven lifespan extension in vertebrates: a meta-analysis. Aging Cell https://doi.org/10.1111/acel.70131 (2025).
Soda, K., Dobashi, Y., Kano, Y., Tsujinaka, S. & Konishi, F. Polyamine-rich food decreases age-associated pathology and mortality in aged mice. Exp. Gerontol. 44, 727–732 (2009).
Hofer, S. J. et al. Spermidine is essential for fasting-mediated autophagy and longevity. Nat. Cell Biol. 26, 1571–1584 (2024).
Eisenberg, T. et al. Cardioprotection and lifespan extension by the natural polyamine spermidine. Nat. Med. 22, 1428–1438 (2016).
Pietrocola, F. et al. Spermidine induces autophagy by inhibiting the acetyltransferase EP300. Cell Death Differ. 22, 509–516 (2015).
Baur, J. A. et al. Resveratrol improves health and survival of mice on a high-calorie diet. Nature 444, 337–342 (2006).
Pearson, K. J. et al. Resveratrol delays age-related deterioration and mimics transcriptional aspects of dietary restriction without extending life span. Cell Metab. 8, 157–168 (2008).
Strong, R. et al. Evaluation of resveratrol, green tea extract, curcumin, oxaloacetic acid, and medium-chain triglyceride oil on life span of genetically heterogeneous mice. J. Gerontol. A Biol. Sci. Med. Sci. 68, 6–16 (2013).
Mercken, E. M. et al. SRT2104 extends survival of male mice on a standard diet and preserves bone and muscle mass. Aging Cell 13, 787–796 (2014).
Mitchell, S. J. et al. The SIRT1 activator SRT1720 extends lifespan and improves health of mice fed a standard diet. Cell Rep. 6, 836–843 (2014).
Boily, G. et al. SirT1 regulates energy metabolism and response to caloric restriction in mice. PLoS ONE 3, e1759 (2008).
Li, Y., Xu, W., McBurney, M. W. & Longo, V. D. SirT1 inhibition reduces IGF-I/IRS-2/Ras/ERK1/2 signaling and protects neurons. Cell Metab. 8, 38–48 (2008).
Mercken, E. M. et al. SIRT1 but not its increased expression is essential for lifespan extension in caloric-restricted mice. Aging Cell 13, 193–196 (2014).
Fang, E. F. et al. NAD+ in aging: molecular mechanisms and translational implications. Trends Mol. Med. 23, 899–916 (2017).
Lautrup, S., Sinclair, D. A., Mattson, M. P. & Fang, E. F. NAD+ in brain aging and neurodegenerative disorders. Cell Metab. 30, 630–655 (2019).
Zhang, J. et al. Emerging strategies, applications and challenges of targeting NAD+ in the clinic. Nat. Aging 5, 1704–1731 (2025).
Zhang, H. et al. NAD+ repletion improves mitochondrial and stem cell function and enhances life span in mice. Science 352, 1436–1443 (2016).
Harrison, D. E. et al. 17-α-estradiol late in life extends lifespan in aging UM-HET3 male mice; nicotinamide riboside and three other drugs do not affect lifespan in either sex. Aging Cell 20, e13328 (2021).
Mills, K. F. et al. Long-term administration of nicotinamide mononucleotide mitigates age-associated physiological decline in mice. Cell Metab. 24, 795–806 (2016).
Mitchell, S. J. et al. Nicotinamide improves aspects of healthspan, but not lifespan, in mice. Cell Metab. 27, 667–676 (2018).
Harrison, D. E. et al. Acarbose improves health and lifespan in aging HET3 mice. Aging Cell 18, e12898 (2019).
Strong, R. et al. Longer lifespan in male mice treated with a weakly estrogenic agonist, an antioxidant, an α-glucosidase inhibitor or a Nrf2-inducer. Aging Cell 15, 872–884 (2016).
Qu, Q. et al. Lithocholic acid phenocopies anti-ageing effects of calorie restriction. Nature https://doi.org/10.1038/s41586-024-08329-5 (2024).
Wilding, J. P. H. et al. Once-weekly semaglutide in adults with overweight or obesity. N. Engl. J. Med. 384, 989–1002 (2021).
Garvey, W. T. et al. Two-year effects of semaglutide in adults with overweight or obesity: the STEP 5 trial. Nat. Med. 28, 2083–2091 (2022).
Lincoff, A. M. et al. Semaglutide and cardiovascular outcomes in obesity without diabetes. N. Engl. J. Med. 389, 2221–2232 (2023).
Holst, J. J. GLP-1 physiology in obesity and development of incretin-based drugs for chronic weight management. Nat. Metab. 6, 1866–1885 (2024).
Johansen, V. B. I. et al. Brain control of energy homeostasis: implications for anti-obesity pharmacotherapy. Cell 188, 4178–4212 (2025).
Secher, A. et al. The arcuate nucleus mediates GLP-1 receptor agonist liraglutide-dependent weight loss. J. Clin. Invest. 124, 4473–4488 (2014).
McMorrow, H. E. et al. Incretin receptor agonism rapidly inhibits AgRP neurons to suppress food intake in mice. J. Clin. Invest. https://doi.org/10.1172/jci186652 (2025).
Friedrichsen, M., Breitschaft, A., Tadayon, S., Wizert, A. & Skovgaard, D. The effect of semaglutide 2.4 mg once weekly on energy intake, appetite, control of eating, and gastric emptying in adults with obesity. Diabetes Obes. Metab. 23, 754–762 (2021).
Petersen, J., Merrild, C., Lund, J., Holm, S. & Clemmensen, C. Lead-in calorie restriction enhances the weight-lowering efficacy of incretin hormone-based pharmacotherapies in mice. Mol. Metab. 89, 102027 (2024).
Ravussin, E. et al. Tirzepatide did not impact metabolic adaptation in people with obesity, but increased fat oxidation. Cell Metab. 37, 1060–1074 (2025).
Wharton, S. et al. Orforglipron, an oral small-molecule GLP-1 receptor agonist for obesity treatment. N. Engl. J. Med. https://doi.org/10.1056/nejmoa2511774 (2025).
Sonne, N. et al. 2182-LB: development and characterization of a humanized GLP-1 receptor mouse model for the evaluation of small-molecule GLP1R agonists. Diabetes 74, 2182-LB (2025).
Wang, A. & Speakman, J. R. Potential downsides of calorie restriction. Nat. Rev. Endocrinol. https://doi.org/10.1038/s41574-025-01111-1 (2025).
Aw, D., Silva, A. B. & Palmer, D. B. Immunosenescence: emerging challenges for an ageing population. Immunology 120, 435–446 (2007).
Pawelec, G. Age and immunity: what is “immunosenescence”? Exp. Gerontol. 105, 4–9 (2018).
Gerbase-DeLima, M., Liu, R. K., Cheney, K. E., Mickey, R. & Walford, R. L. Immune function and survival in a long-lived mouse strain subjected to undernutrition. Gerontology 21, 184–202 (1975).
Nikolich-Žugich, J. & Messaoudi, I. Mice and flies and monkeys too: caloric restriction rejuvenates the aging immune system of non-human primates. Exp. Gerontol. 40, 884–893 (2005).
Ingram, D. K. & de Cabo, R. Calorie restriction in rodents: caveats to consider. Ageing Res. Rev. 39, 15–28 (2017).
Roecker, E. B., Kemnitz, J. W., Ershler, W. B. & Weindruch, R. Reduced immune responses in Rhesus monkeys subjected to dietary restriction. J. Gerontol. A Biol. Sci. Med. Sci. 51A, B276–B279 (1996).
Sun, D., Muthukumar, A. R., Lawrence, R. A. & Fernandes, G. Effects of calorie restriction on polymicrobial peritonitis induced by cecum ligation and puncture in young C57BL/6 mice. Clin. Diagn. Lab. Immunol. 8, 1003–1011 (2001).
Kang, W., Saito, H., Fukatsu, K., Hidemura, A. & Matsuda, T. Diet restriction impairs extracellular signal-regulated kinase activation of peritoneal exudative cells after N-formyl-methionyl-leucyl-phenylalanine stimulation in a murine peritonitis model. JPEN J. Parenter. Enteral Nutr. 26, 259–264 (2002).
Starr, M. E., Steele, A. M., Cohen, D. A. & Saito, H. Short-term dietary restriction rescues mice from lethal abdominal sepsis and endotoxemia and reduces the inflammatory/coagulant potential of adipose tissue. Crit. Care Med. 44, e509–e519 (2016).
Hasegawa, A. et al. Alternate day calorie restriction improves systemic inflammation in a mouse model of sepsis induced by cecal ligation and puncture. J. Surg. Res. 174, 136–141 (2012).
Peck, M. D., Babcock, G. F. & Alexander, J. W. The role of protein and calorie restriction in outcome from salmonella infection in mice. JPEN J. Parenter. Enteral Nutr. 16, 561–565 (1992).
Trujillo-Ferrara, J. et al. Caloric restriction increases free radicals and inducible nitric oxide synthase expression in mice infected with Salmonella typhimurium. Biosci. Rep. 31, 273–282 (2011).
Murray, M., Murray, A., Murray, N. & Murray, M. Diet and cerebral malaria: the effect of famine and refeeding. Am. J. Clin. Nutr. 31, 57–61 (1978).
Hunt, N. H., Manduci, N. & Thumwood, C. M. Amelioration of murine cerebral malaria by dietary restriction. Parasitology 107, 471–476 (1993).
Mejia, P. et al. Dietary restriction protects against experimental cerebral malaria via leptin modulation and T-cell mTORC1 suppression. Nat. Commun. 6, 6050 (2015).
Gardner, E. M. Caloric restriction decreases survival of aged mice in response to primary influenza infection. J. Gerontol. A Biol. Sci. Med. Sci. 60, 688–694 (2005).
Ritz, B. W., Aktan, I., Nogusa, S. & Gardner, E. M. Energy restriction impairs natural killer cell function and increases the severity of influenza infection in young adult male C57BL/6 mice. J. Nutr. 138, 2269–2275 (2008).
Clinthorne, J. F., Adams, D. J., Fenton, J. I., Ritz, B. W. & Gardner, E. M. Short-term re-feeding of previously energy-restricted C57BL/6 male mice restores body weight and body fat and attenuates the decline in natural killer cell function after primary influenza infection. J. Nutr. 140, 1495–1501 (2010).
Goldberg, E. L. et al. Lifespan-extending caloric restriction or mTOR inhibition impair adaptive immunity of old mice by distinct mechanisms. Aging Cell 14, 130–138 (2015).
Beura, L. K. et al. Normalizing the environment recapitulates adult human immune traits in laboratory mice. Nature 532, 512–516 (2016).
Reiser, K., McGee, C., Rucker, R. & McDonald, R. Effects of aging and caloric restriction on extracellular matrix biosynthesis in a model of injury repair in rats. J. Gerontol. A Biol. Sci. Med. Sci. 50A, B40–B47 (1995).
Emery, P. W. & Sanderson, P. Effect of dietary restriction on protein synthesis and wound healing after surgery in the rat. Clin. Sci. 89, 383–388 (1995).
Otranto, M., Souza-Netto, I., guila, M. B. & Monte-Alto-Costa, A. Male and female rats with severe protein restriction present delayed wound healing. Appl. Physiol. Nutr. Metab. 34, 1023–1031 (2009).
Reed, M. J. et al. Enhanced cell proliferation and biosynthesis mediate improved wound repair in refed, caloric-restricted mice. Mech. Ageing Dev. 89, 21–43 (1996).
Hunt, N. D. et al. Effect of calorie restriction and refeeding on skin wound healing in the rat. Age 34, 1453–1458 (2012).
Roth, G. S. et al. Effect of age and caloric restriction on cutaneous wound closure in rats and monkeys. J. Gerontol. A Biol. Sci. Med. Sci. 52A, B98–B102 (1997).
Forni, M. F. et al. Caloric restriction promotes structural and metabolic changes in the skin. Cell Rep. 20, 2678–2692 (2017).
Chen, H. et al. Intermittent fasting triggers interorgan communication to suppress hair follicle regeneration. Cell 188, 157–174 (2025).
Harvie, M. N. et al. The effects of intermittent or continuous energy restriction on weight loss and metabolic disease risk markers: a randomized trial in young overweight women. Int. J. Obes. 35, 714–727 (2011).
Liu, D. et al. Calorie restriction with or without time-restricted eating in weight loss. New Engl. J. Med. 386, 1495–1504 (2022).
Dote-Montero, M. et al. Effects of early, late and self-selected time-restricted eating on visceral adipose tissue and cardiometabolic health in participants with overweight or obesity: a randomized controlled trial. Nat. Med. 31, 524–533 (2025).
Blackwell, B. -N., Bucci, T. J., Hart, R. W. & Turturro, A. Longevity, body weight, and neoplasia in ad libitum-fed and diet-restricted C57BL6 mice fed NIH-31 open formula diet. Toxicol. Pathol. 23, 570–582 (1995).
Moreschi, C. Beziehungen zwischen Ernährung und Tumorwachstum. Zeitschrift für Immunitaetsforschung 2, 651–675 (1909).
Rous, P. The influence of diet on transplanted and spontaneous mouse tumors. J. Exp. Med. 20, 433–451 (1914).
Tannenbaum, A. The initiation and growth of tumors: introduction. I. Effects of underfeeding. Am. J. Cancer 38, 335–350 (1940).
Xie, K. et al. Every-other-day feeding extends lifespan but fails to delay many symptoms of aging in mice. Nat. Commun. 8, 155 (2017).
Olshansky, S., Carnes, B. & Cassel, C. In search of Methuselah: estimating the upper limits to human longevity. Science 250, 634–640 (1990).
Olshansky, S. J. & Carnes, B. A. Inconvenient truths about human longevity. J. Gerontol. A Biol. Sci. Med. Sci. 74, S7–S12 (2019).
Konno, A., Hishinuma, K., Hashimoto, Y., Kimura, S. & Nishimura, T. Dietary restriction reduces the incidence of 3-methylcholanthrene-induced tumors in mice: close correlation with its potentiating effect on host T cell functions. Cancer Immunol. Immunother. 33, 293–298 (1991).
Kolaja, K. L., Bunting, K. A. & Klaunig, J. E. Inhibition of tumor promotion and hepatocellular growth by dietary restriction in mice. Carcinogenesis 17, 1657–1664 (1996).
Nogueira, L. M. et al. Dose-dependent effects of calorie restriction on gene expression, metabolism, and tumor progression are partially mediated by insulin-like growth factor-1. Cancer Med. 1, 275–288 (2012).
Harvey, A. E. et al. Calorie restriction decreases murine and human pancreatic tumor cell growth, nuclear factor-κB activation, and inflammation-related gene expression in an insulin-like growth factor-1−dependent manner. PLoS ONE 9, e94151 (2014).
Novelle, M. G. et al. Caloric restriction induces heat shock response and inhibits B16F10 cell tumorigenesis both in vitro and in vivo. Aging 7, 233–239 (2015).
Pomatto-Watson, L. C. D. et al. Daily caloric restriction limits tumor growth more effectively than caloric cycling regardless of dietary composition. Nat. Commun. 12, 6201 (2021).
Seyfried, B. T. N., Kiebish, M., Marsh, J. & Mukherjee, P. Targeting energy metabolism in brain cancer through calorie restriction and the ketogenic diet. J. Cancer Res. Ther. 5, 7–15 (2009).
Vernieri, C. et al. Fasting-mimicking diet is safe and reshapes metabolism and antitumor immunity in patients with cancer. Cancer Discov. 12, 90–107 (2022).
Udumula, M. P. et al. Intermittent fasting induced ketogenesis inhibits mouse epithelial ovarian cancer by promoting antitumor T cell response. iScience 26, 107839 (2023).
Hursting, S. D., Perkins, S. N. & Phang, J. M. Calorie restriction delays spontaneous tumorigenesis in p53-knockout transgenic mice. Proc. Natl Acad. Sci. USA 91, 7036–7040 (1994).
Vernieri, C., Ligorio, F., Tripathy, D. & Longo, V. D. Cyclic fasting-mimicking diet in cancer treatment: preclinical and clinical evidence. Cell Metab. 36, 1644–1667 (2024).
Ingram, D. K., Weindruch, R., Spangler, E. L., Freeman, J. R. & Walford, R. L. Dietary restriction benefits learning and motor performance of aged mice. J. Gerontol. 42, 78–81 (1987).
Kapogiannis, D. et al. Brain responses to intermittent fasting and the healthy living diet in older adults. Cell Metab. 36, 1668–1678 (2024).
Prehn, K. et al. Caloric restriction in older adults—differential effects of weight loss and reduced weight on brain structure and function. Cereb. Cortex 27, 1765–1778 (2017).
Martin, C. K. et al. Examination of cognitive function during six months of calorie restriction results of a randomized controlled trial. Rejuvenation Res. 10, 179–190 (2007).
Wang, J. et al. Caloric restriction attenuates β-amyloid neuropathology in a mouse model of Alzheimer’s disease. FASEB J. 19, 1–18 (2005).
Patel, N. V. et al. Caloric restriction attenuates Aβ-deposition in Alzheimer transgenic models. Neurobiol. Aging 26, 995–1000 (2005).
Mouton, P. R., Chachich, M. E., Quigley, C., Spangler, E. & Ingram, D. K. Caloric restriction attenuates amyloid deposition in middle-aged dtg APP/PS1 mice. Neurosci. Lett. 464, 184–187 (2009).
Zhang, J. et al. Intermittent fasting protects against Alzheimer’s disease possible through restoring aquaporin-4 polarity. Front. Mol. Neurosci. 10, 395 (2017).
Halagappa, V. K. M. et al. Intermittent fasting and caloric restriction ameliorate age-related behavioral deficits in the triple-transgenic mouse model of Alzheimer’s disease. Neurobiol. Dis. 26, 212–220 (2007).
Babygirija, R. et al. Fasting is required for many of the benefits of calorie restriction in the 3xTg mouse model of Alzheimer’s disease. Nat. Commun. 16, 7147 (2025).
Lazic, D. et al. Every-other-day feeding exacerbates inflammation and neuronal deficits in 5XFAD mouse model of Alzheimer’s disease. Neurobiol. Dis. 136, 104745 (2020).
Pan, R. -Y. et al. Intermittent fasting protects against Alzheimer’s disease in mice by altering metabolism through remodeling of the gut microbiota. Nat. Aging 2, 1024–1039 (2022).
Qin, W. et al. Calorie restriction attenuates Alzheimer’s disease type brain amyloidosis in squirrel monkeys (Saimiri sciureus). J. Alzheimer’s Dis. 10, 417–422 (2006).
Liu, Y. et al. SIRT3 mediates hippocampal synaptic adaptations to intermittent fasting and ameliorates deficits in APP mutant mice. Nat. Commun. 10, 1886 (2019).
Rubovitch, V. et al. Dietary energy restriction ameliorates cognitive impairment in a mouse model of traumatic brain injury. J. Mol. Neurosci. 67, 613–621 (2019).
Whittaker, D. S. et al. Circadian modulation by time-restricted feeding rescues brain pathology and improves memory in mouse models of Alzheimer’s disease. Cell Metab. 35, 1704–1721 (2023).
Cogut, V., McNeely, T. L., Bussian, T. J., Graves, S. I. & Baker, D. J. Caloric restriction improves spatial learning deficits in tau mice. J. Alzheimer’s Dis. 98, 925–940 (2024).
Bruce-Keller, A. J., Umberger, G., McFall, R. & Mattson, M. P. Food restriction reduces brain damage and improves behavioral outcome following excitotoxic and metabolic insults. Ann. Neurol. 45, 8–15 (1999).
Duan, W. & Mattson, M. P. Dietary restriction and 2-deoxyglucose administration improve behavioral outcome and reduce degeneration of dopaminergic neurons in models of Parkinson’s disease. J. Neurosci. Res. 57, 195–206 (1999).
Yu, Z. F. & Mattson, M. P. Dietary restriction and 2-deoxyglucose administration reduce focal ischemic brain damage and improve behavioral outcome: evidence for a preconditioning mechanism. J. Neurosci. Res. 57, 830–839 (1999).
Fitzgerald, K. C. et al. Effect of intermittent vs. daily calorie restriction on changes in weight and patient-reported outcomes in people with multiple sclerosis. Mult. Scler. Relat. Disord. 23, 33–39 (2018).
Fitzgerald, K. C. et al. Intermittent calorie restriction alters T cell subsets and metabolic markers in people with multiple sclerosis. eBioMedicine 82, 104124 (2022).
Strøm, A. & Jensen, R. A. Mortality from circulatory diseases in Norway 1940–1945. Lancet 257, 126–129 (1951).
Fontana, L., Meyer, T. E., Klein, S. & Holloszy, J. O. Long-term calorie restriction is highly effective in reducing the risk for atherosclerosis in humans. Proc. Natl Acad. Sci. USA 101, 6659–6663 (2004).
Fortmann, S. P., Haskell, W. L., Wood, P. D. & Team, S. W. C. P. Effects of weight loss on clinic and ambulatory blood pressure in normotensive men. Am. J. Cardiol. 62, 89–93 (1988).
Caviezel, F. et al. Early improvement of left ventricular function during caloric restriction in obesity. Int. J. Obes. 10, 421–426 (1986).
Wan, R., Camandola, S. & Mattson, M. P. Intermittent fasting and dietary supplementation with 2-deoxy-D-glucose improve functional and metabolic cardiovascular risk factors in rats. FASEB J. 17, 1133–1134 (2003).
Mager, D. E. et al. Caloric restriction and intermittent fasting alter spectral measures of heart rate and blood pressure variability in rats. FASEB J. 20, 631–637 (2006).
Broderick, T. L., Driedzic, W. R., Gillis, M., Jacob, J. & Belke, T. Effects of chronic food restriction and exercise training on the recovery of cardiac function following ischemia. J. Gerontol. A Biol. Sci. Med. Sci. 56, B33–B37 (2001).
Ahmet, I., Wan, R., Mattson, M. P., Lakatta, E. G. & Talan, M. Cardioprotection by intermittent fasting in rats. Circulation 112, 3115–3121 (2005).
Katare, R. G., Kakinuma, Y., Arikawa, M., Yamasaki, F. & Sato, T. Chronic intermittent fasting improves the survival following large myocardial ischemia by activation of BDNF/VEGF/PI3K signaling pathway. J. Mol. Cell. Cardiol. 46, 405–412 (2009).
Dutzmann, J. et al. Intermittent fasting after ST-segment–elevation myocardial infarction improves left ventricular function: the randomized controlled INTERFAST-MI trial. Circ. Heart Fail. 17, e010936 (2024).
Piper, M. D. W., Partridge, L., Raubenheimer, D. & Simpson, S. J. Dietary restriction and aging: a unifying perspective. Cell Metab. 14, 154–160 (2011).
Partridge, L., Fuentealba, M. & Kennedy, B. K. The quest to slow ageing through drug discovery. Nat. Rev. Drug Discov. 19, 513–532 (2020).
Fang, E. F. et al. A research agenda for ageing in China in the 21st century (2nd edition): focusing on basic and translational research, long-term care, policy and social networks. Ageing Res. Rev. 64, 101174 (2020).
Fang, E. F. et al. Adapting health, economic and social policies to address population aging in China. Nat. Aging 5, 2176–2187 (2025).
Lane, M. A. et al. Dietary restriction in nonhuman primates: progress report on the NIA study. Ann. N. Y. Acad. Sci. 673, 36–45 (1992).
Ramsey, J. J. et al. Dietary restriction and aging in rhesus monkeys: the University of Wisconsin study. Exp. Gerontol. 35, 1131–1149 (2000).
Dal-Pan, A. et al. Caloric restriction or resveratrol supplementation and ageing in a non-human primate: first-year outcome of the RESTRIKAL study in Microcebus murinus. Age 33, 15–31 (2011).
Kaneko, T., Tahara, S. & Matsuo, M. Retarding effect of dietary restriction on the accumulation of 8-hydroxy-2′-deoxyguanosine in organs of Fischer 344 rats during aging. Free Radic. Biol. Med. 23, 76–81 (1997).
Kisby, G. E. et al. Effect of caloric restriction on base-excision repair (BER) in the aging rat brain. Exp. Gerontol. 45, 208–216 (2010).
Vera, E., Jesus, B. B. de, Foronda, M., Flores, J. M. & Blasco, M. A. Telomerase reverse transcriptase synergizes with calorie restriction to increase health span and extend mouse longevity. PLoS ONE 8, e53760 (2013).
Hass, B. S., Hart, R. W., Lu, M. H. & Lyn-Cook, B. D. Effects of caloric restriction in animals on cellular function, oncogene expression, and DNA methylation in vitro. Mutat. Res. 295, 281–289 (1993).
Cohen, H. Y. et al. Calorie restriction promotes mammalian cell survival by inducing the SIRT1 deacetylase. Science 305, 390–392 (2004).
Hahn, O. et al. Dietary restriction protects from age-associated DNA methylation and induces epigenetic reprogramming of lipid metabolism. Genome Biol. 18, 56 (2017).
Bonelli, M. A. et al. Low-level caloric restriction rescues proteasome activity and Hsc70 level in liver of aged rats. Biogerontology 9, 1–10 (2008).
Ntsapi, C. M. & Loos, B. Neurons die with heightened but functional macro- and chaperone mediated autophagy upon increased amyloid-ß induced toxicity with region-specific protection in prolonged intermittent fasting. Exp. Cell. Res. 408, 112840 (2021).
Cerletti, M., Jang, Y. C., Finley, L. W. S., Haigis, M. C. & Wagers, A. J. Short-term calorie restriction enhances skeletal muscle stem cell function. Cell Stem Cell 10, 515–519 (2012).
Fontana, L. et al. The effects of graded caloric restriction: XII. Comparison of mouse to human impact on cellular senescence in the colon. Aging Cell 17, e12746 (2018).
Bareja, A. et al. Liver-derived plasminogen mediates muscle stem cell expansion during caloric restriction through the plasminogen receptor Plg-RKT. Cell Rep. 43, 113881 (2024).
Deepa, S. S., Unnikrishnan, A., Matyi, S., Hadad, N. & Richardson, A. Necroptosis increases with age and is reduced by dietary restriction. Aging Cell 17, e12770 (2018).
Sbierski-Kind, J. et al. Effects of caloric restriction on the gut microbiome are linked with immune senescence. Microbiome 10, 57 (2022).
de França, N. A. G., Rolland, Y., Guyonnet, S. & de Barreto, P. S. The role of dietary strategies in the modulation of hallmarks of aging. Ageing Res. Rev. 87, 101908 (2023).
Speakman, J. R., Mitchell, S. E. & Mazidi, M. Calories or protein? The effect of dietary restriction on lifespan in rodents is explained by calories alone. Exp. Gerontol. 86, 28–38 (2016).
Harper, J. M., Leathers, C. W. & Austad, S. N. Does caloric restriction extend life in wild mice? Aging Cell 5, 441–449 (2006).
Green, C. L. et al. Sex and genetic background define the metabolic, physiologic, and molecular response to protein restriction. Cell Metab. 34, 209–226 (2022).
Heydari, A. R., Wu, B., Takahashi, R., Strong, R. & Richardson, A. Expression of heat shock protein 70 is altered by age and diet at the level of transcription. Mol. Cell. Biol. 13, 2909–2918 (1993).
HALL, D. M. et al. Caloric restriction improves thermotolerance and reduces hyperthermia-induced cellular damage in old rats. FASEB J. 14, 78–86 (2000).
McCay, C. M., Maynard, L. A., Sperling, G. & Barnes, L. L. Retarded growth, life span, ultimate body size and age changes in the albino rat after feeding diets restricted in calories four figures. J. Nutr. 18, 1–13 (1939).
Campbell, B. A. & Richardson, R. Effect of chronic undernutrition on susceptibility to cold stress in young adult and aged rats. Mech. Ageing Dev. 44, 193–202 (1988).
Talan, M. I. & Ingram, D. K. Effect of intermittent feeding on thermoregulatory abilities of young and aged C57BL/6J mice. Arch. Gerontol. Geriatr. 4, 251–259 (1985).
First Appeared on
Source link






