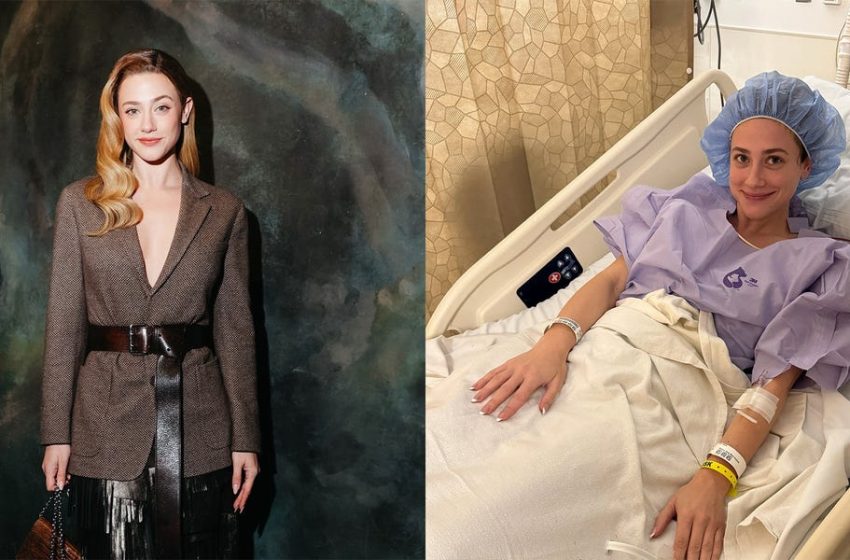
Lili Reinhart on Her Yearlong Journey to an Endometriosis Diagnosis
I was sitting in a bathtub at 4 A.M., in the summer of 2024, wondering if I should go to the emergency room after eight straight hours of UTI-like symptoms. A warm bath felt like my last attempt at relief before taking an Uber to a hospital in Cologne, Germany, where I was filming an independent movie.
After a few hours at the hospital, the results came back as a mild infection. I left with amoxicillin, went back to my hotel and finally slept. But it wasn’t over—and it wouldn’t be for over a year. That day was only the beginning of a long, intense journey toward a diagnosis.
I filmed the entirety of the movie with constant urinary urgency and frequency. I returned to the hospital and was given more antibiotics. Doctors shrugged at me, seemingly less invested because I wasn’t a permanent resident. An ultrasound ruled out cysts. I called physicians back home for advice, to no avail. For five long weeks, no one could help me. I relied on my mom and boyfriend for emotional support via text and posted daily on my Instagram “Close Friends,” sharing miserable health updates with my inner circle.
The movie wrapped, and on the 12-hour flight home, I was seated far away from the bathroom. I took a Xanax and waited for it to kick in, making six trips to the toilet before I could sleep. Unfortunately, anti-anxiety medication was the only thing that allowed me to rest at that point, the only thing that quieted the urgency to pee that crept up on me every three to five minutes. After that experience, flying became an intense trigger of anxiety for me—something that still exists to this day.
I went straight from the airport to a urologist in Los Angeles, suitcases in tow, where I had my first catheter inserted. I held back tears through the pinching discomfort and texted my mom afterward saying that I couldn’t believe this was still happening to my body. Although painful, I felt this was finally a step toward relief now that I was back home.
But the urine culture came back negative—it wasn’t a UTI, and the relief I’d imagined quickly disappeared.
I pushed through the following months, surviving on AZO and Xanax, waiting for an appointment with a urogynecologist. I went back to the hospital again, afraid I was missing a possibly dangerous infection that could reach my kidneys. They sent me home with no answers.
Somehow, I traveled to Europe twice during this period, at the height of my discomfort. I remember stepping off a boat in Venice during the film festival, in full glam and a gown, thinking: If only any of these people knew how I felt right now. I found it strangely amusing that my pain was invisible from the outside. I smiled and posed and socialized, quietly stepping away when it didn’t seem suspicious to use the restroom. I became acutely aware of how strange it looked to excuse myself so often. This led me to hold in the discomfort for longer than I should have, just to avoid raising eyebrows.
After months of searching, interstitial cystitis became the prime suspect. I began a six-week series of bladder instillations: weekly catheter insertions, followed by steroids injected directly into my bladder. During one of my last sessions, the catheter wasn’t placed far enough inside my bladder. When I stood up, the medication spilled down my legs and onto the floor. I stuck my head out the door, calling out my doctor’s name. She had to do the instillation again. When symptoms didn’t improve, we did a cystoscopy of my bladder, which showed inflammation, but no concrete answers.
Relief finally came through pelvic floor therapy. Each session would alleviate my symptoms for one or two days. So I attended weekly sessions for months, until work took me out of town again.
During one session, my pelvic floor therapist asked me if I had ever considered endometriosis as a cause of my symptoms. None of the eight or so doctors I had seen before her had mentioned it. I hesitantly brought it up to my urogynecologist, not wanting to be dismissed. She seemed neutral about it, but gave me the name of a doctor who specialized in minimally invasive gynecologic care. I had an ultrasound, before being sent for an MRI.
The results came in a few days later while I was on my way back from getting blood drawn: “Adenomyosis. No endometriosis detected.” I Googled the word “adenomyosis” and was stopped cold by a symptom listed: infertility. I had no plans to become pregnant within the next few years, but I know I want kids eventually and suddenly the desires I had for my future felt disrupted. I went home, woke up my boyfriend, and cried in his arms. He asked me what happened, but I didn’t have the words or energy to explain it in the moment. He just held me while I cried through my pain, confusion, and frustration.
I had a follow-up call with my doctor about the diagnosis, where she casually claimed, “Usually women will get a hysterectomy to manage their pain.” I was 28. And I didn’t even have the classic symptoms of adenomyosis—none of this made sense as a cause of my persistent bladder pain.
My pelvic floor therapist encouraged me to pursue a conversation with an endometriosis surgeon to get more information. I had been poked, prodded, examined, pinched, and catheterized—I could barely stand the idea of another pair of blue gloves coming near me. This was on top of a growing resentment toward doctors who weren’t covered by insurance, had long wait lists, and offered no solutions. I was entering my fifth year of a long health journey that began post-COVID. Blood panels and gut maps consistently showed inflammation, but I was never given a definitive autoimmune diagnosis.
I had an 80-minute appointment with an endometriosis surgeon and, after our conversation and pelvic exam, he recommended laparoscopic surgery for a diagnosis, and excision of endometriosis if found. I went to see my gynecologist again, who warned me that my surgery might find nothing at all. The notion of waking up after surgery and being told it was all for nothing became my biggest fear. She also added that endometriosis often grows back and, since I was now interested in freezing my eggs, the estrogen injections were likely to cause me to flare all over again. I tried not to cry in her office.
She suggested the birth control pill. I had switched to an IUD years ago due to suspicions that the pill was affecting my weight and mood. My psychiatrist also warned that the pill had a 40 percent chance of making my already chronic depression even worse. But I had taken my IUD out months earlier on the off-chance that it was contributing to my bladder issues and was enjoying being hormone-free ever since. I left the doctor’s office feeling like the pill was being offered to quiet my problem—not solve it.
I spent the rest of the spring and all summer of 2025 considering whether surgery was something I wanted to pursue. I met with another surgeon for a second opinion, where I was told surgery was not necessary and that I should just go on birth control to manage my symptoms.
I think it’s important to note that I’ve never been someone who settles for band-aid solutions. If there is an underlying issue, I want to find it. Not later, or eventually, but now. I would not stop until I had answers.
My endometriosis surgeon was patient with me, and when I was feeling cold feet toward laparoscopy, he performed another pelvic exam at my request. His opinion on surgery stayed the same.
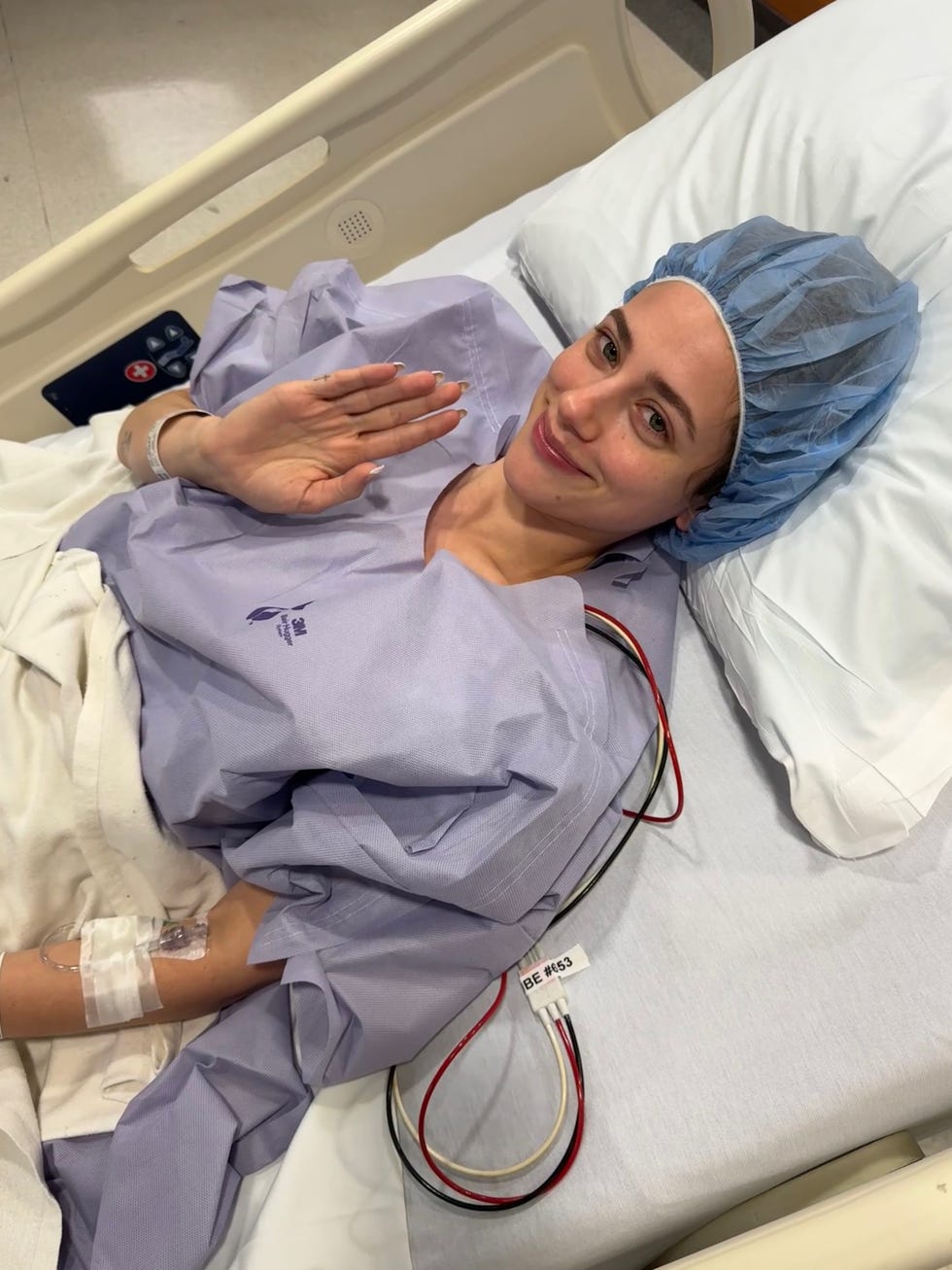
I woke up at 3:50 A.M. on December 4. My boyfriend drove us to the hospital for a 5 A.M. intake. I felt calm and ready. Knowing I would be intubated, I asked if I could bring lip balm into the operating room; I didn’t want to wake up with chapped lips. The anesthesiologist laughed and said no one had ever asked that before.
As I groggily woke up after the operation, my surgeon sat at the end of my bed. My words were slurred, but I asked, “Did you find it?”
“We found endometriosis,” he replied.
In an instant, I felt validated. My pain, discomfort, and suffering for over a year was no longer an unknown question.
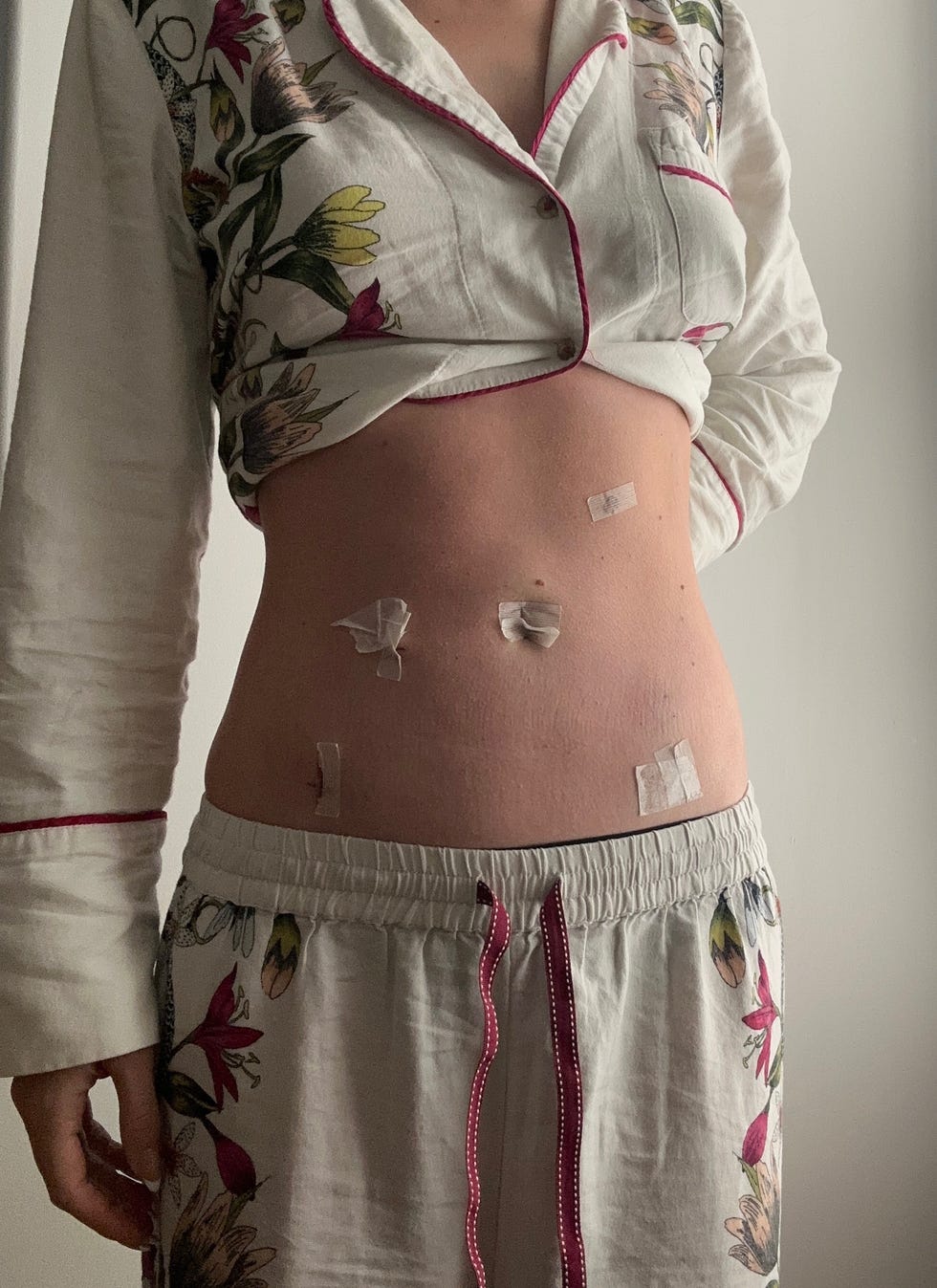
I went home with confirmed diagnoses of endometriosis and adenomyosis. My surgical photos were stapled together with pen marks circling the visible disease, including an unexpected cyst that was removed, along with two hernias. They also removed my appendix. I spent the following days on the couch, medicated, drifting in and out of sleep with my boyfriend and dog beside me. Thankfully, I was well enough to travel home for the holidays to see my family.
I posted about my diagnosis on Instagram and opened the floodgates to thousands of women DM’ing and texting me about their similar experiences. Sharing my experience led to a friend finally getting a diagnosis herself from my surgeon after being ignored by countless other doctors. It’s heartbreaking and disturbing to see how universally women’s pain is ignored and pushed aside. I was lucky that my diagnosis didn’t take multiple years, which it often does.
I don’t know what lies ahead in the years to come in terms of my relationship with this disease, my fertility, or bladder pain. But I do know that I wasn’t exaggerating my discomfort or imagining my pain. What was happening to my body was very real, and I deserved to be taken seriously much sooner than I was.
Women’s pain is not an inconvenience and should never be treated that way. The purpose of sharing my experience is to encourage and uplift other women who may be experiencing pain, to not be silenced into accepting it as the norm. Self-advocacy can lead you somewhere, so please keep going.
First Appeared on
Source link