
Ozempic-Like Drugs Can Help You Lose Weight, But There’s a Catch : ScienceAlert
A new analysis suggests that people who stop taking Ozempic-like medications keep off about 25 percent of the weight they lost, up to a year later. But here’s the catch: it’s not known how much of this weight loss is muscle rather than fat.
This medical mystery highlights an underexplored consequence of semaglutide, tirzepatide, and other drugs prescribed to manage type 2 diabetes or body weight. Some initial studies indicate that 40 to 60 percent of the weight lost during treatment may constitute lean muscle mass.
While it’s well documented that patients regain weight after discontinuing these medications, it’s not clear what the pounds are comprised of.
“If the regained weight is disproportionately fat, individuals may ultimately be worse off than before in their fat-to-lean mass ratio, which may have adverse consequences for their health,” explains medical researcher Brajan Budini, co-first author of the study by a team at the University of Cambridge in the UK.
Their published paper provides a comprehensive review of the evidence on post-cessation weight gain, and is also the first to model its trajectory up to 52 weeks after treatment cessation.
Weight management after stopping treatment is important, as over a billion people live with obesity worldwide. GLP-1 drugs have demonstrated great efficacy, sometimes helping individuals achieve body weight reductions of 20 percent or more.
The medications mimic a natural hormone called glucagon-like peptide-1 (GLP-1), which helps to control blood sugar and reduce appetite. Yet due to gastrointestinal and other side effects, as well as steep prices or prescription complications, about half of patients stop using GLP-1 drugs within the first year.
“Drugs such as Ozempic and Wegovy act like brakes on our appetite, making us feel full sooner, which means we eat less and therefore lose weight,” says Budini.
“When people stop taking them, they are essentially taking their foot off the brake, and this can lead to rapid weight regain.”
To model how much weight patients regain after ceasing treatment, the researchers examined 48 relevant studies. Their limitations and inconsistencies soon became apparent.
Some studies tracked patient weight outcomes only for a few weeks, and there was significant variability in when patients were followed up with after stopping medication. Overall, post-GLP-1 weight gain “has been largely underexplored in the literature,” the authors say.
Therefore, the researchers chose only a handful of high-quality publications that met certain criteria. These studies had to be randomized, include more than 100 participants each, report weight loss of at least 3 kilograms (6.6 pounds), and include at least one check-up 12 weeks after medication was stopped.
As a result, they filtered their systematic review to just six randomized controlled trials (RCTs) comprising more than 3,200 people. These especially rigorous studies followed participants for up to 52 weeks after discontinuing weight-loss drugs.
This (somewhat mini) meta-analysis revealed that post-GLP-1 patients experienced a rapid initial weight regain that gradually slowed. A year after stopping the medications, they regained 60 percent of the weight they had lost during treatment.
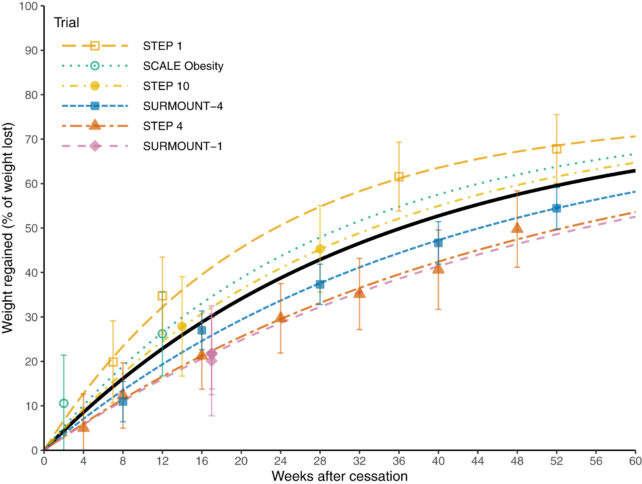
The researchers then used this data to predict the effects beyond 52 weeks. They projected that weight regain begins to plateau at 60 weeks and tapers off after patients regain 75 percent of the weight lost during treatment. But why?
It’s possible that the medications help patients form healthier eating habits or induce physiological changes, such as altering hormone levels or hypothalamic function.
However, a sizable portion of lost weight is muscle, and it’s uncertain if lean mass recovers as quickly as fat mass after treatment. Furthermore, newer, more effective drugs like semaglutide and tirzepatide are less effective in preserving lean mass – that is, they facilitate greater weight reduction regardless of its source.
Related: Sudden Sight Loss Risk Almost 5x Higher With Wegovy Than Ozempic, Study Finds
Therefore, prescription strategies that taper doses could help patients at least maintain fat loss. It’s also helpful for physicians to encourage patients to adopt healthy eating and exercise, which are vital for sustained well-being.
“It’s important that people are given advice on improving their diet and exercise, rather than relying solely on the drugs, as this may help them maintain good habits when they stop taking them,” concludes medical researcher and co-first author Steven Luo.
This research was published in eClinicalMedicine.
First Appeared on
Source link






