
The new face of America’s deadliest cancer: Fit, healthy young people are being diagnosed in record numbers… now concerned experts believe they have uncovered why
For decades, it has worn the same, unmistakable face: that of a lifelong smoker. But the profile of lung cancer is beginning to change.
Lung cancer remains the leading cause of cancer deaths in the US, representing about a fifth of the total and accounting for approximately 125,000 fatalities every year.
Smoking is tied to about 80 percent of cases. But the share in nonsmokers is rising – from eight percent in the early 1990s to 20 percent by 2022.
In its early stages, symptoms are vague and easily dismissed: a persistent cough that does not go away, mild back or joint pain, unexplained fatigue, or coughing up blood – even small amounts – that stops as quickly as it starts.
As more nonsmokers receive the devastating diagnosis, doctors are racing to identify the drivers.
Environmental pollution and toxic chemicals are increasingly under scrutiny. Air pollution not only irritates the lungs but also alters the way genes function.
Breathing in fine particle pollution increases a nonsmoker’s risk of developing lung cancer by eight percent and dying from it by 11 percent.
Exposure to pollution, coupled with certain genetic faults, appears to trigger cancer, according to experts.
Long before her diagnosis, Laura Reed dealt with a persistent morning cough, episodes of coughing up blood, and years of lower back and wrist pain. She brushed off the symptoms as stress, allergies, or simply getting older
‘Studies suggest that lung cancer in never-smokers may have different genetic mutations, such as in the EGFR gene, compared to smokers,’ Dr Nabil Rizk, Chief of Thoracic Surgery at Hackensack University Medical Center in New Jersey, told the Daily Mail. ‘Air pollution is a notable risk factor for lung cancer in this group.’
For Laura Reed, the possibility of lung cancer never crossed her mind.
She was vigilant about her health, undergoing colonoscopies due to her mother’s death from colorectal cancer at 38, alongside cervical cancer screenings and mammograms driven by concern about her risk.
A nonsmoker, she also followed a healthy diet and exercised regularly. And because she had never smoked, lung cancer screening – which involves a CT scan – was never on her radar.
Long before her diagnosis, Reed had symptoms: a persistent morning cough, episodes of coughing up blood, and years of lower back and wrist pain.
She brushed them off as stress, allergies, or simply getting older.
Reed took every preventative step possible, but they were no match for the toxic pollution she was exposed to while serving in the Navy overseas.
When she was diagnosed with stage IV lung cancer at 37, she and her doctors came to believe that exposure during her service could have been the culprit.
She first noticed something was wrong about a year before her diagnosis, with a persistent cough, mostly in the mornings.
There were several times she coughed up blood, but she dismissed it as stress, allergies, or the price of being too busy to slow down.
She also had lower back pain she had been battling for years and wrist pain she assumed was arthritis. At 37, she was active, ate well, and never smoked. None of it added up to cancer in her mind.
But these are all warning signs of lung cancer – often vague, easily dismissed, or mistaken for less serious conditions.
‘Symptoms of lung cancer in never-smokers, such as a persistent cough, back pain, joint pain, or coughing up blood, are often dismissed because they are non-specific and can be attributed to more common, benign causes. This can lead to a delayed diagnosis,’ Rizk said.
‘A never-smoker should seek further medical investigation for any persistent and unexplained symptoms, including a cough that doesn’t go away or worsens, chest pain, shortness of breath, wheezing, hoarseness, unexplained weight loss, or coughing up blood.’
Reed, who served in the Navy as a nuclear surface warfare officer in her 20s, went to her closest VA hospital in North Charleston in April 2023 for her regular annual checkup.
She was expecting the usual: blood work, a few questions, and a clean bill of health.

Reed had never smoked, so screening for the disease was not on her radar. Years later, she believes exposure to toxic pollution during her service, including burn pits in the Persian Gulf, may have triggered the cancer that would be diagnosed at stage IV
But this time was different. Her wrists hurt. Her lower back ached. And then there was the cough.
For the wrist pain, her doctor handed her arthritis cream, attributing the soreness to getting older. But when Reed mentioned the year-long cough, the doctor’s tone shifted.
‘That’s highly unusual,’ she recalls being told.
She was quickly sent for an X-ray, which found a six-millimeter nodule in her lung. She was reassured that service members get lung nodules all the time and there was no need to panic – just follow up with a CT scan.
Lung nodules are common among veterans, particularly in the Navy, often due to long-term exposure to asbestos on ships, as well as diesel exhaust, jet fuel, and other airborne hazards.
Service members deployed overseas breathe in desert dust, burn pit smoke, secondhand tobacco smoke, and explosion debris. At the height of the Iraq and Afghanistan wars, the military burned 200 to 400 tons of waste per day.
The Department of Defense estimates 3.5 million service members were exposed to burn pit emissions.
Reed had never smoked, so screening for the disease was not on her radar. Years later, she believes exposure to toxic pollution during her service, including burn pits in the Persian Gulf, may have triggered the cancer.

Shira Boehler, 44, from Nashville, Tennessee, described herself as ‘healthy’ and ‘very active’ before she was diagnosed with lung cancer last fall
Rizk said: ‘Military burn pits, used extensively in Iraq and Afghanistan, released a hazardous mix of substances, including particulate matter, benzene, and other carcinogens. This exposure is a major concern for veterans’ respiratory health.
‘The Department of Veterans Affairs has established a list of ‘presumptive conditions’ related to airborne hazards and burn pit exposure, which includes various lung cancers.’
Reed went home after the X-ray and did what anyone would do – she Googled her symptoms.
Everything she read seemed benign. Cancer came up as a possibility, but she pushed that thought aside. Not cancer. That was not going to happen to her.
She got the CT scan a few days later. She was driving away from the facility when her phone rang.
‘It’s never good when they call you that fast,’ she said.
The doctor’s voice was calm but grave. The six-millimeter nodule was actually a six-centimeter mass – ten times larger than first thought.
Reed had stage IV cancer.

She got surgery in October, during which doctors removed part of her right lung, and she was declared officially cancer free afterward

She had ‘no symptoms’ and no family history of lung cancer, and she only caught the cancer because she had decided to get a full–body MRI as someone who values her health
‘I was just in shock for the longest time,’ she said. ‘I didn’t even have the stereotype thinking-wise. I’ve never smoked tobacco before. I was just like, how did I get this?’
Reed is far from alone.
Shira Boehler, 44, from Nashville, described herself as ‘healthy’ and ‘very active’ before she was diagnosed with lung cancer last fall.
A non-smoker who ran six miles daily, she discovered the disease only by chance – after opting for a full-body MRI as a proactive health measure.
‘I did a preventative scan because I thought it would be good to have a baseline look. I felt strong and healthy and had no symptoms,’ she told the Daily Mail.
‘I have never ever smoked a single puff of a cigarette. I’m a proud never-smoker.’
The scan found a 3.8cm mass in her lung.
Like Reed, she had no family history, no lifestyle red flags, and no warning signs until the scan revealed otherwise.

Dr Nabil Rizk, Chief of Thoracic Surgery at Hackensack University Medical Center in New Jersey , told the Daily Mail that never-smokers often dismiss lung cancer symptoms, including cough, back pain and coughing up blood, as harmless, causing dangerous delays
Radiologists initially told her not to worry given her lack of symptoms. Still, she showed the scan to her pulmonologist father and a doctor friend.
Both said she could get a low-dose CT scan – the gold-standard screening test – if she wanted peace of mind. At first, she brushed it off. Then she reconsidered.
On September 26, 2025, she went for her first scan. The tumor had grown.
Three days later came a more detailed scan, followed by a procedure in which a doctor threaded a scope into her lungs to take a tissue sample.
The results came back on October 1: stage 1B adenocarcinoma.
She had no symptoms and no family history – and only caught the cancer because she chose to get a scan.
She underwent surgery in October to remove part of her right lung and was declared cancer-free.
Two months after surgery, she was back to running six miles a day.
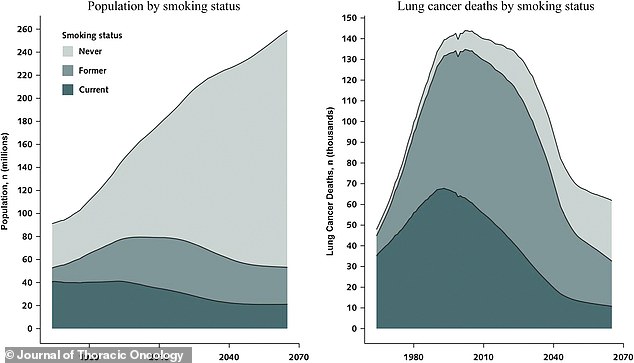
The left side shows that as the smoking population shrinks and ages out, the never-smoking population grows and ages. The right side shows that by approximately 2040–2065, more lung cancer deaths will occur in people who have never smoked or who formerly smoked than in current smokers
‘I feel like the luckiest girl in the world,’ she said. ‘But cancer doesn’t care. If you have lungs, you can get lung cancer. It is not a deserved disease.’
Unlike Boehler, whose cancer was caught early, Reed’s disease was discovered much later – at stage IV.
For Boehler, the trigger remains unknown. For Reed, the likely cause was exposure to carcinogens during her military service.
In Reed’s case, those exposures may have flipped the ‘on’ switch in a gene that had been in her DNA since birth but was inactive.
That gene is ALK (anaplastic lymphoma kinase). When switched on, it tells lung cells to grow and divide uncontrollably.
‘Environmental factors could play a role. Some research has found a positive correlation between estimated ALK fusion frequency in [non-small cell lung cancer] and high levels of indoor radon exposure,’ Rizk said.
‘While it’s not definitively proven that exposures like burn pit smoke, diesel exhaust or sulfur dioxide directly trigger the ALK mutation, they are known carcinogens that can increase the overall risk of developing lung cancer.
‘It is plausible that these exposures could contribute to the genetic changes that lead to ALK-positive lung cancer.’

Now 40, Reed rides horses and plays mahjong with friends twice a week. A daily targeted therapy pill – a TKI – has turned her aggressive ALK-positive lung cancer into a manageable chronic disease. Her tumor ‘melted away,’ her pain vanished and she says she feels like she’s in her 20s again
Genetic mutations such as EGFR, ALK, and ROS1 are more common in never-smokers, particularly women, appearing in up to 80 to 90 percent of some groups.
Unlike the lung cancer most people picture, these forms often strike younger, otherwise healthy adults – often women in their 30s and 40s. There is no routine screening and no clear prevention.
The standard low-dose CT screening is reserved for older adults with heavy smoking histories – meaning patients like Reed do not qualify.
Rizk said: ‘With regards to the screening guidelines, there is a growing debate about whether they should be expanded.
‘Some studies suggest that extending screening to high-risk never-smokers, such as those with a family history of lung cancer, could be beneficial.
‘There is no consensus on a specific age or symptom threshold for offering low-dose CT scans to never-smokers, and more research is needed to establish clear guidelines.’
But there is a silver lining.
Targeted therapy pills called tyrosine kinase inhibitors (TKIs) can shut that broken switch off, turning an aggressive cancer into a manageable chronic disease.
For patients like Reed, these drugs have given her years she was never supposed to have.
Before targeted therapies, stage IV lung cancer was a death sentence measured in months. Chemotherapy bought some time, but the cancer always returned.
The treatment is a daily pill that targets the faulty gene – without chemo or radiation.
The results were immediate. Her cough disappeared. Her back pain vanished. Her tumor ‘melted away,’ and she felt young again.
Now 40, Reed rides horses and plays mahjong with friends twice a week. A daily TKI has transformed her disease into a manageable condition.
‘My joint pain has pretty much gone away since starting the medication,’ she said. ‘That’s why I say I feel like I’m in my 20s again, because in my 30s, I’ve just been in pain all the time.’
When Reed was diagnosed at 37, the average survival for ALK-positive patients on modern TKIs was seven to ten years – a significant improvement from the months patients once faced.
She knows she will not live as long as she would have without cancer. She is hoping for ten years.
She rides horses. She plays mahjong. She has turned 40. None of this time was guaranteed, and she is determined to make the most of it.
The good news is that awareness and screening policies can change.
Expanding screening beyond smoking history could catch more cases earlier. Better recognition of symptoms like persistent cough, back pain, and unexplained fatigue could speed diagnosis. Wider access to genetic testing could identify mutations such as ALK, EGFR, and ROS1 earlier, opening the door to targeted therapies.
Research into environmental exposures – particularly for veterans exposed to burn pits – may also help identify the triggers behind these cancers and inform prevention strategies.
Because lung cancer is no longer just a smoker’s disease.
First Appeared on
Source link






