The Silent Killer Hidden in Plain Sight, And Your Hand Holds the Clue
Acromegaly affects roughly 8 to 24 people per 100,000 and, when left untreated, cuts life expectancy by approximately a decade. Despite its severity, the condition is notoriously difficult to catch early: its symptoms, enlarged hands and feet, headaches, gradual facial changes, develop so slowly that patients often don’t notice them. According to the study published in The Journal of Clinical Endocrinology & Metabolism, around 24% of patients currently experience diagnostic delays exceeding ten years.
What makes this research particularly notable is not just its accuracy, but its design philosophy. By deliberately avoiding facial images and fingerprints, the Kobe University team built a tool that could realistically be deployed in public health checkups or primary care clinics without triggering the privacy concerns that have stalled earlier AI diagnostic approaches.
A Model Trained on Over 11,000 Hand Images
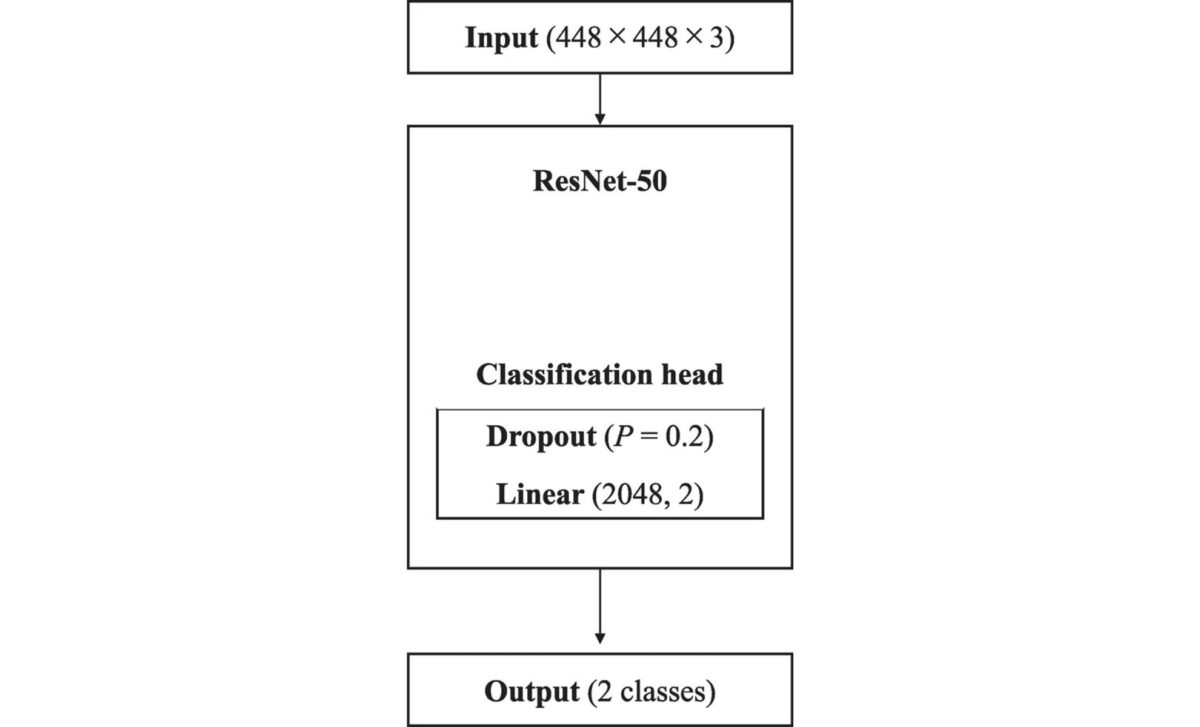
The study enrolled 716 patients, 317 with confirmed acromegaly and 399 controls, drawn from 15 medical facilities across Japan. According to the researchers, more than 11,000 hand images were collected and used to train and validate a deep learning model built on a ResNet-50 architecture, a well-established framework for image classification tasks.
Two specific hand positions were captured: a dorsal (back-of-hand) view with fingers extended, and a clenched fist with the thumb on the outside. The latter position was chosen partly because of a known clinical phenomenon called the “fist sign“, the inability of acromegaly patients to cover their fingernails with the center of their palm when clenching, which has long been recognized anecdotally but never formally validated as a diagnostic marker.
The dataset was divided at the facility level, with roughly 80% of patients assigned to training and validation, and 20% held back for testing. This institutional separation was designed to rigorously test whether the model could generalize beyond the centers that trained it.
Outperforming Human Specialists
At its optimal decision threshold, the AI model achieved a sensitivity of 0.89, a specificity of 0.91, a positive predictive value of 0.88, and a negative predictive value of 0.93. Its area under the ROC curve hit 0.96, a figure that indicates near-excellent overall discrimination between patients with and without the condition.
Ten board-certified endocrinologists with an average of nearly a decade of experience were given the same test images. According to the study‘s comparative analysis, their F1 scores, a combined measure of precision and recall, ranged from 0.43 to 0.63, well below the model’s F1 score of 0.89.
Gradient-weighted Class Activation Mapping, a visualization technique applied to the model’s outputs, suggested that it focused its attention on finger joints, fingernails in the clenched fist position, and the region near the base of the thumb, areas consistent with the physical manifestations of the disease rather than incidental background features.
Privacy by Design, Scalability by Intent
One of the most deliberate aspects of the study was its approach to anonymization. Unlike prior AI diagnostic tools that relied on facial photographs, raising obvious identification concerns, this model was restricted entirely to dorsal hand and fist images captured against uniform backgrounds with no personally identifying elements. According to the authors, this “privacy-by-design” strategy reduces compliance burdens and legal risks, making deployment in public settings far more feasible.
First author Yuka Ohmachi, a graduate student at Kobe University, noted that achieving this level of diagnostic performance without facial features was unexpected. Lead researcher Hidenori Fukuoka emphasized that the model’s value lies not in replacing specialists, but in extending diagnostic reach: endocrinologists rely on voice changes, facial expressions, biochemical markers, and full medical histories, none of which a hand photo can capture.
The research team acknowledged meaningful limitations, including the fact that most acromegaly patients in the dataset had already received treatment, potentially reducing the visibility of physical signs. The model was also trained exclusively on Japanese patients, and its generalizability to other ethnic groups and community settings remains to be established through external validation.
First Appeared on
Source link






