Japan Approves the World’s First Treatments Made With Reprogrammed Human Cells
Japan has cleared two therapies that began with the same lab technique and ended in very different parts of the body. One is placed on the surface of the heart. The other is injected deep into the brain. Together, they became the first approved medical products in the world made from reprogrammed human cells, pushing iPS cells into real clinical use after years of research and testing.
The approval did not create instant mass access. The products were granted conditional, time-limited authorization by Japan’s Ministry of Health, Labour, and Welfare, which means both therapies still have to keep proving safety and effectiveness after approval. In practical terms, iPS cell treatment has entered the medical system, but under scrutiny.
The story also runs through one name that has shaped the field from the start: Shinya Yamanaka of Kyoto University. In comments cited by WIRED, Yamanaka said, “We are very pleased to have taken a major step toward social implementation on the 20th anniversary of the announcement of mouse iPS cells.” He added, “To establish this as a medical treatment, it is essential to go through the process of confirming its safety and efficacy in many more cases.”
Two Approved Therapies Started from the Same Cell Platform
The two products share a scientific origin in induced pluripotent stem cells, but they target different diseases and use different delivery methods. ReHeart, developed by Cuorips, is aimed at patients with severe heart failure caused by ischemic cardiomyopathy. Amshepli, also referred to as laguneprocel, was developed by Sumitomo Pharma and RACTHERA for people with Parkinson’s disease whose symptoms are not adequately controlled by existing drug therapy, including levodopa.
This is where the phrase reprogrammed human cells matters. iPS cells are adult cells that have been reset into a flexible state so they can be guided into other cell types. That makes them central to regenerative medicine and stem cell therapy, two terms that now connect directly to approved products rather than distant research goals.
The approval also reflects a system Japan spent years building. The supply chain includes research institutions, manufacturing sites, university hospitals, and the Kyoto University iPS Cell Research Foundation, which helps provide clinical-grade cell stocks for use in therapy development. Japan’s domestic infrastructure is one reason the first commercial approvals happened there rather than elsewhere.
The Heart Therapy Was Built for Patients with Few Options Left
For ReHeart, the medical need is blunt. Patients with advanced heart failure who do not improve enough with standard treatment may face a shrinking set of options, including heart transplant or mechanical support devices. Those routes are limited by donor shortages, age restrictions, infection risk, and the long-term burden of living with invasive hardware.
The treatment itself is not a full heart replacement. During open-chest surgery, doctors place three sheets of cardiomyocytes derived from iPS cells onto the heart’s surface. According to the source material, the transplanted cells are expected to release cytokines that promote angiogenesis and repair ischemic areas through a paracrine effect, helping improve the condition of the heart muscle.
The early data were small, but they were strong enough for regulators to let the product move forward. In a multicenter Japanese study of eight patients, four showed a trend toward improvement, with peak VO2 rising by more than 10% at 52 weeks after transplant. Japan now plans a post-approval outcomes study targeting 75 patients, with sales expected around the fall of 2026.
The company’s own framing is also tightly tied to first-of-its-kind status. On its homepage, Cuorips says it aims to contribute to medicine through research, development, and manufacturing centered on the world’s first iPS cell-derived cardiomyocyte sheets. That language matches the way the approval has been presented across the Japanese sources: not as a finished endpoint, but as the first commercial opening for heart failure treatment built from iPS cells.
The Parkinson’s Treatment Took a More Direct Path Into the Brain
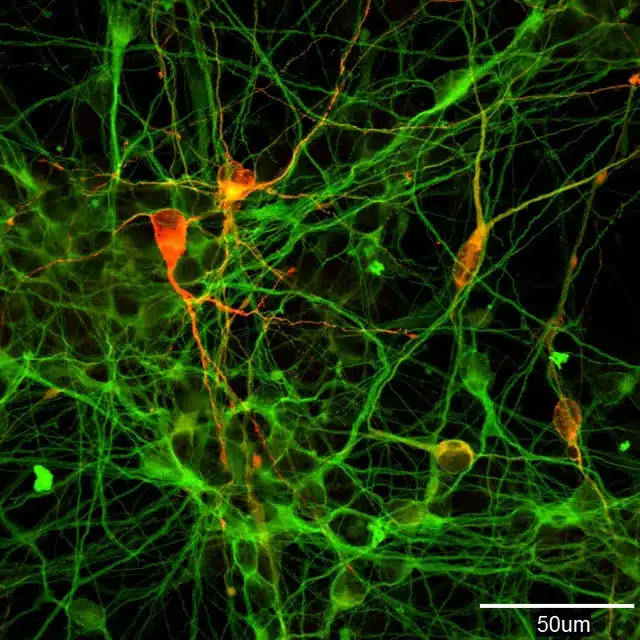
The second therapy, Amshepli, addresses a different kind of damage. Parkinson’s disease gradually reduces dopamine-producing neurons in the brain, leading to tremor, rigidity, and other motor symptoms. Existing medications can ease those symptoms, but they do not replace the lost nerve cells, which is why this approach tries to put new progenitor cells directly where they are needed.
The procedure uses stereotactic brain surgery. Surgeons make small openings in the skull and inject the cells into both sides of the brain through multiple delivery tracks. In the physician-led trial at Kyoto University Hospital, four of six evaluable patients showed improvement in MDS-UPDRS Part III motor scores 24 months after transplantation, and the reports said graft survival was confirmed in all six cases.
That result was enough to push the product into restricted use, but researchers have been careful not to oversell what happened. Jun Takahashi, the CiRA director who led the Parkinson’s trial, said, “The results of the deliberations are a major step forward, but even if approval is granted, that is not the goal, but only the beginning of new medicine.” The line captures the tone of Japan’s approval system, where commercial use begins before the scientific debate is fully closed.
Japan’s health minister also framed the approval in explicitly national terms. At a press conference cited by WIRED, Kenichiro Ueno said, “I am very pleased that a therapeutic product from Japan based on Professor Yamanaka’s iPS cells has been put into practical use for the first time in the world.” That statement helps explain why Japan’s approval of iPS cell treatments is likely to become one of the strongest Google Discover phrases around this story: it combines a national first, a medical milestone, and a search-ready breakthrough in regenerative medicine.
Approval Was a Breakthrough, but Access Will Still Take Time
The approval does not mean every eligible patient can receive these therapies right away. The Japanese sources say the products still need further steps tied to insurance coverage and post-marketing data collection before they can reach broader clinical use. That makes this less a final arrival than the start of a supervised commercial phase for iPS cell therapy in the real world.
Twenty years after mouse iPS cells were first reported, Japan now has approved products made from reprogrammed human cells for heart failure treatment and Parkinson’s treatment, with both therapies still required to gather long-term evidence under conditional approval.
First Appeared on
Source link






